Seeing the term “actinic damage” on a skin biopsy report can raise immediate questions. Is it serious? Does it mean cancer? Is there something you need to do next?
At Honest Pathology, we regularly help patients walk through reports like this so they can clearly understand what’s being said. Actinic damage on your pathology report is a very common finding, especially in people with a history of sun exposure, but the wording can feel vague without context.
The good news is that once you understand what actinic damage actually represents, it becomes much easier to interpret what it means for your skin and your health.
What Is Actinic Damage?
Actinic damage refers to changes in the skin caused by long-term exposure to ultraviolet (UV) light, primarily from the sun. Over time, this exposure affects the structure of the skin at both the surface and deeper levels.
Rather than being a single condition, actinic damage is a broad term that describes a spectrum of changes. These can range from mild sun-related alterations to more advanced precancerous changes.
When a pathologist uses this term, they are identifying evidence that the skin has been affected by cumulative sun exposure. It’s essentially a record of how your skin has responded to UV light over the years.
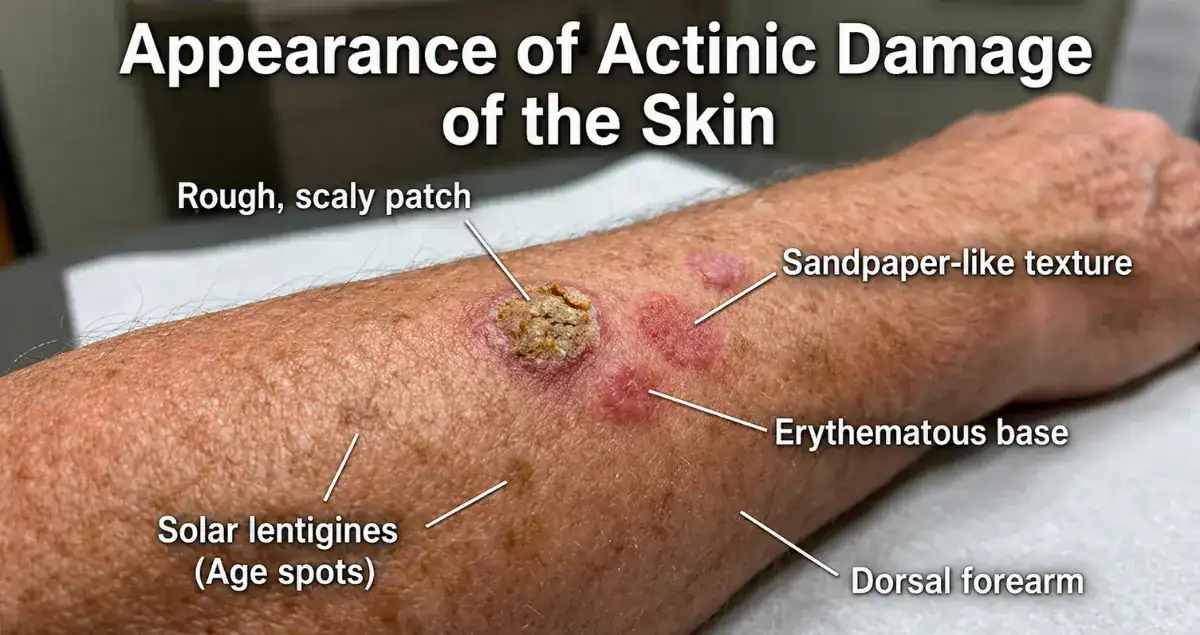
What Does Actinic Damage Look Like on the Skin?
On the surface, actinic damage can show up in a variety of ways.
Some people notice rough, scaly patches that feel dry or slightly gritty. Others may see areas of uneven pigmentation, with lighter or darker spots developing over time. Fine lines, thinning skin, and a loss of elasticity are also common features of sun-damaged skin.
In certain cases, actinic damage appears as more defined lesions, such as actinic keratoses. These are small, rough spots that can be easier to feel than to see and are considered early precancerous changes.
These visible signs are often what lead to a biopsy, especially when a spot looks different from the surrounding skin or doesn’t heal as expected.
What Does It Look Like Under the Microscope?
When we review reports with patients at Honest Pathology, one of the most helpful things is explaining what the pathologist actually saw under the microscope.
Actinic damage has several recognizable features. The outer layer of the skin may show disorganized or abnormal-looking cells, reflecting the effects of UV exposure. In some cases, these changes are mild, while in others they may show early signs of precancerous transformation.
Deeper in the skin, the connective tissue often appears altered. One of the hallmark findings is something called solar elastosis, where the normal supportive fibers are replaced by damaged, thickened material due to chronic sun exposure.
Blood vessels may also appear more prominent or irregular, and the overall structure of the skin can look less uniform than healthy, protected skin.
These microscopic findings help confirm that the changes seen on the surface are related to sun damage.
Is Actinic Damage the Same as Skin Cancer?
One of the most common concerns people have is whether actinic damage means cancer.
The answer is no. Actinic damage itself is not skin cancer. However, it is important because it reflects an environment where skin cancer is more likely to develop over time.
Think of it as a warning sign rather than a diagnosis. Skin that shows actinic damage has been exposed to enough UV radiation to increase the risk of conditions like basal cell carcinoma, squamous cell carcinoma, and, less commonly, melanoma.
In some cases, a biopsy may show both actinic damage and a specific lesion, such as an actinic keratosis or an early skin cancer. In others, it may only show background sun damage without any cancer present.
What About Actinic Keratosis?
Actinic keratosis is closely related to actinic damage and often comes up in the same conversation.
While actinic damage describes a general pattern of sun-related changes, actinic keratosis refers to a specific type of precancerous lesion. These spots have abnormal cells, and while not all of them progress, actinic keratoses can sometimes turn into cancer if left untreated.
Not all actinic keratoses progress to cancer, but they are considered important to identify and manage. This is why dermatologists often treat them even when they are small or not causing symptoms.
Understanding the difference between general actinic damage and a defined lesion like actinic keratosis is an important part of interpreting your report.
Why This Finding Is So Common
Actinic damage is one of the most frequently reported findings in skin biopsies, especially in adults who have spent significant time outdoors.
Areas like the face, scalp, ears, and arms are particularly prone to these changes because they receive the most sun exposure over a lifetime.
Many people are surprised to learn how much cumulative sun exposure affects the skin, even if they haven’t had severe sunburns. The effects build gradually, often becoming more noticeable with age.
The Questions Most People Are Thinking About
When people see “actinic damage” on their report, they’re often trying to answer a few key questions.
They want to know if it’s serious. In most cases, it’s not dangerous on its own, but it does signal an increased risk environment for future skin changes.
They wonder if it can be reversed. Some visible effects of sun damage can improve with treatment and sun protection, but many of the underlying changes are long-lasting.
They ask whether it means they’ll get skin cancer. It doesn’t guarantee that, but it does mean regular skin monitoring becomes more important.
And they often want to know what to do next. That answer depends on whether there are specific lesions present and what your doctor recommends based on your overall skin health.
What You Can Do Moving Forward
If your report mentions actinic damage, it’s an opportunity to take a more proactive approach to your skin.
Sun protection becomes especially important, including the use of sunscreen, protective clothing, and avoiding peak UV hours when possible. Regular skin checks, both at home and with a healthcare provider, can help catch any new or changing spots early.
If specific lesions like actinic keratoses are present, your doctor may recommend treatments to remove or reduce them.
Understanding Your Report Makes All the Difference
Medical language can sometimes make common findings feel more alarming than they are. That’s why taking the time to understand your pathology report is so valuable. If the wording still feels unclear, a pathology consultation can help explain what your report means in plain language.
At Honest Pathology, we help patients review their reports in plain language so they can clearly understand what terms like “actinic damage” actually mean. We don’t change the diagnosis, but we make sure you’re not left guessing about it.
Because when you understand what your skin has been through and what your report is telling you, you’re in a much better position to take control of your skin health and make informed decisions going forward.