Seeing the phrase “lichenoid reaction” in a pathology report can leave you with more questions than answers. It sounds like a diagnosis, but it doesn’t quite explain what’s going on with your skin or what you should do next. At Honest Pathology, this is exactly the kind of situation we help patients navigate—by reviewing reports together and making sure you actually understand your pathology report, what they say and what they don’t say.
Because the truth is, a lichenoid skin reaction is not a final answer. It’s a pattern. And once you understand that, everything starts to make more sense.
What “Lichenoid Reaction” Really Means
When a pathologist uses the term “lichenoid reaction,” they’re describing a specific pattern of inflammation in the skin. This inflammation is focused on a very thin but important area where the top layer of your skin meets the layer underneath.
Think of it as a boundary line. In this pattern, your immune system is active right along that line, causing irritation and damage to the cells that normally sit there. Under the microscope, this creates a recognizable appearance that pathologists are trained to identify.
But here’s the important part: this term doesn’t tell you the exact cause. It tells you what the skin looks like under the microscope, not why it looks that way.
What You Might Notice on Your Skin
Even before a biopsy is done, lichenoid reactions often have visible signs.
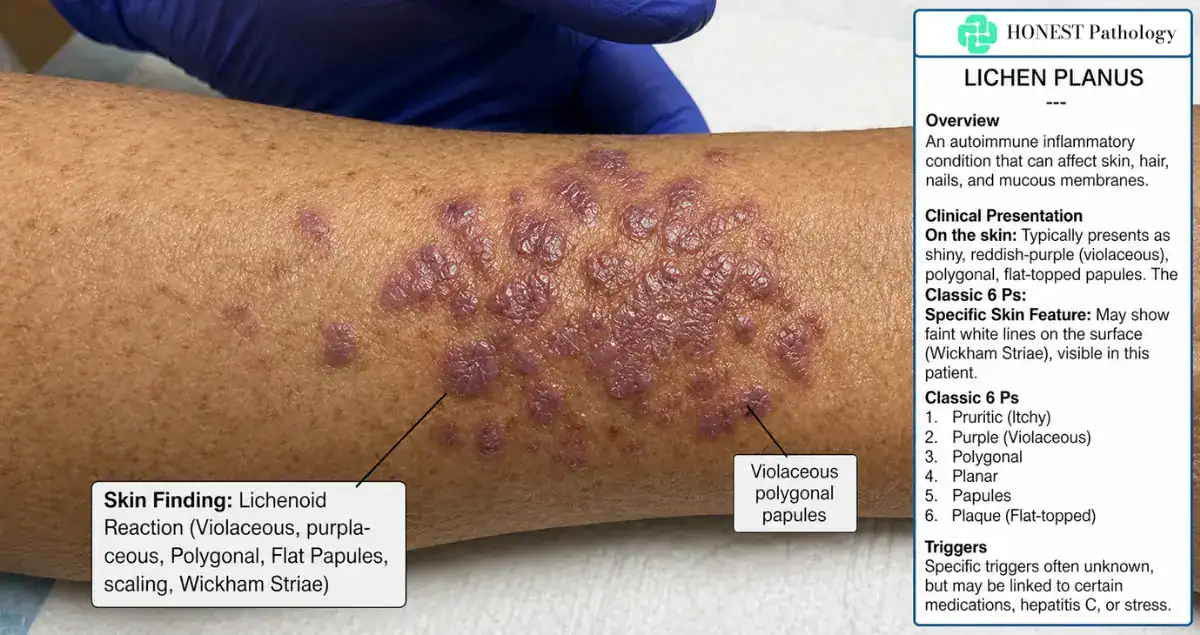
Many people develop small, flat bumps that can look purple, reddish, or darker than their natural skin tone. These spots may be slightly shiny and can feel dry or rough. Itching is very common and sometimes intense.
These changes often show up on areas like the wrists, ankles, or lower back, but they can appear in other places too. Some people notice similar patterns inside the mouth, where they may look like thin white lines, or changes in the nails over time.
Still, these features aren’t exclusive to one condition. That’s why a biopsy is often needed to better understand what’s going on.
What the Biopsy Shows
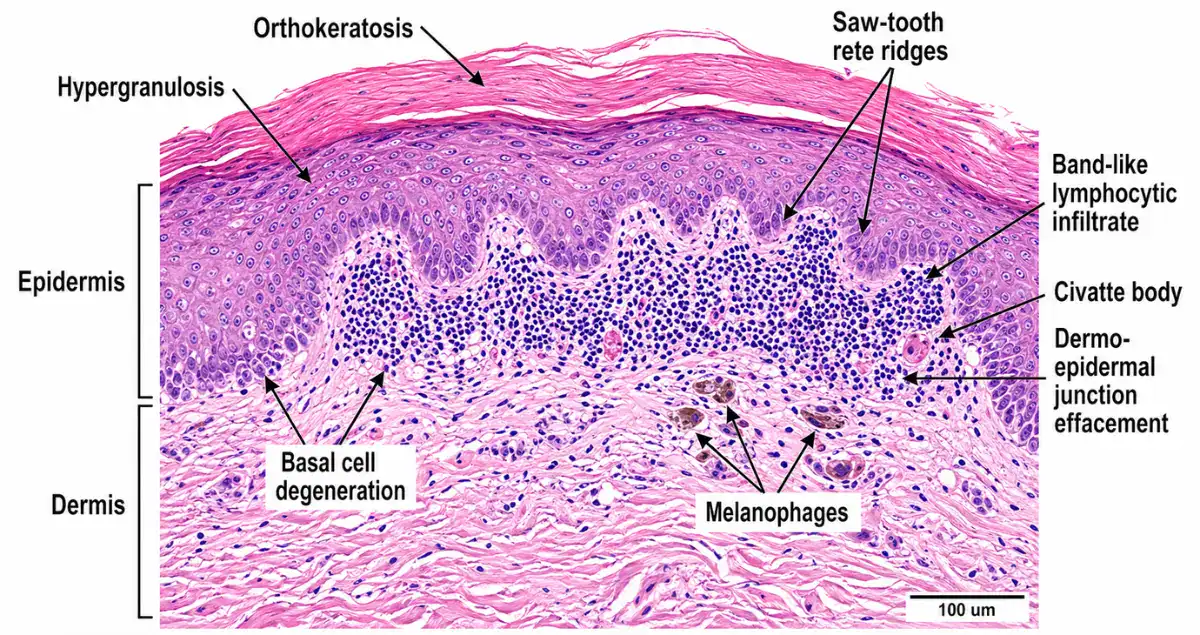
When your skin sample is examined under a microscope, a lichenoid reaction has a few defining features.
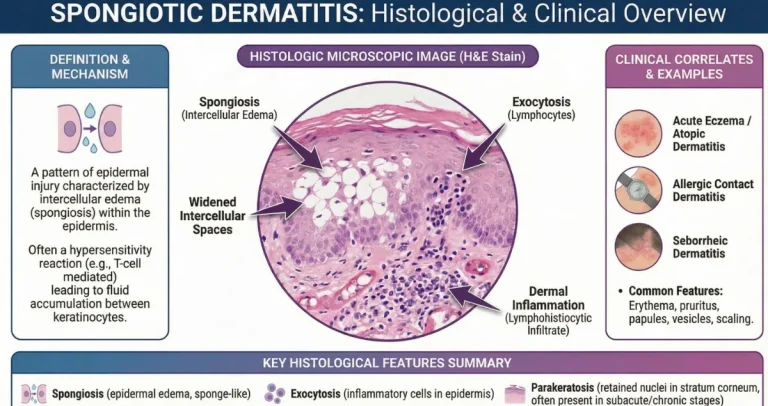
There is typically a layer of immune cells sitting just beneath the surface of the skin, forming a band-like pattern. This tells us that the immune system is actively involved in that specific area.
The cells at the base of the outer skin layer often show signs of damage. Some may look swollen, while others may be breaking down. These changes help confirm the pattern.
The overall structure of the skin can also look slightly different, with a thicker outer layer and a more uneven shape underneath. These microscopic details are what lead to the term “lichenoid reaction” in your report.
The Conditions Most Commonly Linked to This Pattern
Because this is a pattern and not a diagnosis, it can be seen in several different conditions. Some are more common than others, and understanding them can help you better interpret your report.
Lichen planus is one of the most well-known conditions associated with this pattern. It’s an inflammatory skin condition that often causes itchy, flat-topped bumps and follows the classic clinical and microscopic features.
Medications are another common cause. Certain drugs can trigger what’s called a lichenoid drug reaction, which can look very similar to lichen planus both on the skin and under the microscope. In these cases, identifying the connection to a medication is an important step.
Autoimmune conditions like lupus can also produce a lichenoid pattern, as seen in autoimmune disease pathology results where the immune system affects multiple organs, including the skin. Here, the skin findings may be just one part of a larger condition affecting the body.
In people who have had transplants, graft-versus-host disease can also present this way, as the immune system reacts against the skin.
Why the Wording in Your Report Matters
One of the biggest sources of confusion is the language used in pathology reports. Seeing a term like “lichenoid reaction” can feel like you’ve been given a diagnosis, when in reality, it’s only part of the picture.
This is where many people feel stuck. They have a report, but not a clear understanding of what it means for them specifically.
That’s exactly where Honest Pathology comes in. Instead of interpreting or changing your diagnosis, the focus is on reviewing your report with you, line by line if needed, so you can understand the terminology, the level of certainty, and the possible next steps your doctor may consider.
The Questions Most People Are Really Asking
When people see this term, the questions that come up are often the same, even if they’re not always asked directly.
There’s usually concern about how serious it is. In most cases, a lichenoid reaction is not dangerous, but it can be uncomfortable and sometimes long-lasting depending on the cause.
People also want to know if it will go away. Some conditions linked to this pattern can resolve over time, while others may persist or come and go.
Another common concern is whether it’s contagious. It’s not. This type of reaction is driven by the immune system, not an infection.
And of course, many people worry about whether it could be cancer. A lichenoid reaction itself is not cancer, but understanding the full context of your report is important to rule out other possibilities or determine if follow-up is needed.
Understanding Leads to Better Decisions
A pathology report is meant to guide decisions, but it can only do that if it’s understood clearly. When you see a term like “lichenoid reaction,” it’s an invitation to look deeper, not a final answer.
At Honest Pathology, the goal is to help you feel informed and confident when reading your report. By reviewing the findings together, you can better understand what your doctor is considering and what questions to ask next.
Because when you truly understand your pathology, you’re not just reading a report—you’re gaining clarity about your health and taking an active role in your care.