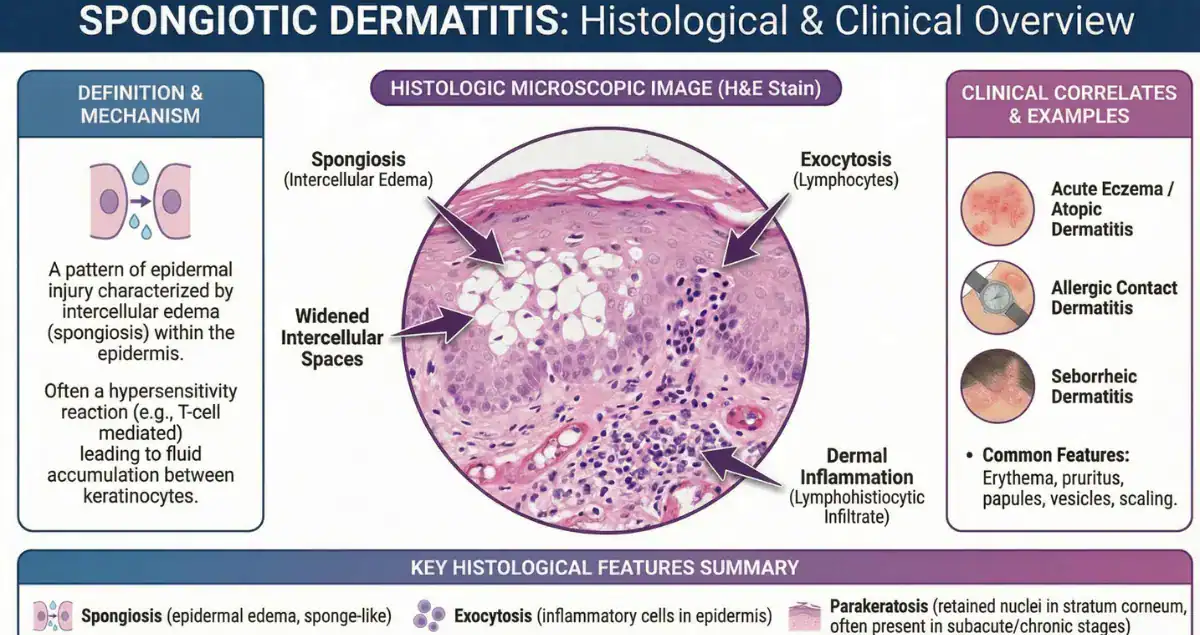
Spongiosis is a very common finding in skin biopsies and refers to a specific type of inflammation within the epidermis, the outermost layer of the skin. While the term may sound unfamiliar or even concerning, it is best understood as a pattern rather than a diagnosis.
At its core, spongiosis describes fluid building up between skin cells. This fluid causes the cells to separate slightly from one another, creating a characteristic appearance under the microscope. It is most often associated with inflammatory skin conditions, especially those that cause itching, redness, or rash.
Importantly, spongiosis does not mean cancer. In fact, it is most commonly seen in benign and treatable skin conditions.
What Does Spongiosis Look Like in Simple Terms?
A helpful way to think about spongiosis is to imagine a dry sponge that has absorbed water. As the sponge fills, small gaps appear between its structure. In the skin, something similar happens when inflammation causes fluid to accumulate between cells.
Under the microscope, pathologists see widened spaces between epidermal cells, with delicate “bridges” still connecting them. In more pronounced cases, tiny fluid-filled spaces called vesicles can form within the skin.
To a patient, this microscopic change often corresponds to visible symptoms like redness, swelling, itching, or even small blisters. While the biopsy shows the pattern, the symptoms are what usually bring someone in for evaluation.
Why Does Spongiosis Happen?
Spongiosis is essentially the skin’s response to irritation or immune activation. When the skin reacts to an allergen, irritant, or internal trigger, inflammatory signals cause fluid to leak into the spaces between cells.
This process is most commonly driven by immune cells, particularly lymphocytes, which move into the skin and release substances that increase vascular permeability. The result is the fluid accumulation that defines spongiosis.
A common question is whether spongiosis is an infection. The answer is no. While infections can sometimes trigger similar reactions, spongiosis itself is not caused by bacteria or viruses. It is a reaction pattern, not a specific disease.
Common Conditions Associated with Spongiosis
Spongiosis is most often associated with a group of conditions broadly referred to as eczematous dermatitis. These are among the most common skin disorders seen in both children and adults.
One of the most frequent causes is atopic dermatitis, often called eczema. In this condition, the skin barrier is impaired, leading to dryness, itching, and inflammation. Biopsies commonly show spongiosis along with a superficial inflammatory infiltrate.
Allergic contact dermatitis is another key diagnosis. This occurs when the skin reacts to a substance such as nickel, fragrances, or certain skincare products. The spongiosis in these cases can be quite prominent and may be accompanied by vesicle formation.
Irritant contact dermatitis produces a similar pattern but is caused by direct damage to the skin rather than an immune-mediated allergic response. Differentiating between these conditions often requires clinical correlation in addition to biopsy findings.
Spongiosis can also be seen in nummular dermatitis, a condition characterized by coin-shaped patches of irritated skin, and in seborrheic dermatitis, which commonly affects the scalp and face.
In some cases, early psoriasis or certain drug reactions may show mild spongiosis, though these conditions usually have additional distinguishing features.
Does Spongiosis Mean Something Serious?
One of the most common concerns is whether spongiosis indicates a serious or chronic condition. In most cases, it does not. It simply reflects inflammation in the skin, which is often manageable and sometimes temporary.
The significance of the finding depends on the underlying cause. For example, allergic contact dermatitis may resolve once the triggering substance is avoided, while atopic dermatitis may be more chronic but still treatable.
Another frequent question is whether spongiosis can turn into cancer. The answer is no. Spongiosis is not a precancerous change and does not increase the risk of skin cancer.
Why a Biopsy Is Helpful
Although many skin conditions can be diagnosed clinically, a biopsy is often performed when the diagnosis is uncertain, the rash is persistent, or treatment has not been effective.
The biopsy allows pathologists to identify patterns like spongiosis and look for additional features that help narrow down the diagnosis. These may include the type of inflammatory cells present, the distribution of changes within the skin layers, and any associated findings such as scaling or thickening.
Patients often ask whether a biopsy can give a definitive answer. In many cases, it provides strong guidance, but the final diagnosis is usually made by combining histologic findings with clinical information.
Why Pathology Reports Can Be Hard to Understand
When patients read a pathology report that mentions spongiosis, it can feel unclear what that actually means for their health. The report may describe microscopic findings without clearly stating the underlying condition.
This can lead to confusion, especially when multiple possible diagnoses are mentioned. Understanding that spongiosis is a pattern not a final diagnosis is an important first step.
Getting Clear Answers with Honest Pathology
This is where Honest Pathology can be especially helpful. Honest Pathology focuses on explaining biopsy results in clear, patient-friendly language, helping individuals understand what findings like spongiosis actually mean.
For example, it can clarify whether the pattern is most consistent with eczema, a contact reaction, or another condition, and explain what features led to that conclusion. This level of explanation helps patients feel more informed and less uncertain.
Instead of trying to interpret technical terminology alone, patients can gain confidence in their diagnosis and better understand their treatment options.
What This Means for Your Skin Health
Spongiosis is one of the most common and recognizable patterns in dermatopathology, and it is usually associated with benign, treatable conditions. While it may sound unfamiliar, it is simply a reflection of how the skin responds to irritation or inflammation.
The key to understanding its significance lies in identifying the underlying cause. With the right diagnosis and treatment, most conditions associated with spongiosis can be effectively managed.
Moving Forward with Confidence
Seeing a term like spongiosis on a pathology report can be confusing, but it is not something to fear. It is a common finding that helps guide diagnosis rather than define a serious disease on its own.
For those seeking clarity, Honest Pathology offers a reliable way to turn complex biopsy findings into understandable insights. With clear explanations and expert interpretation, it becomes much easier to move forward with confidence and take the next steps in care.