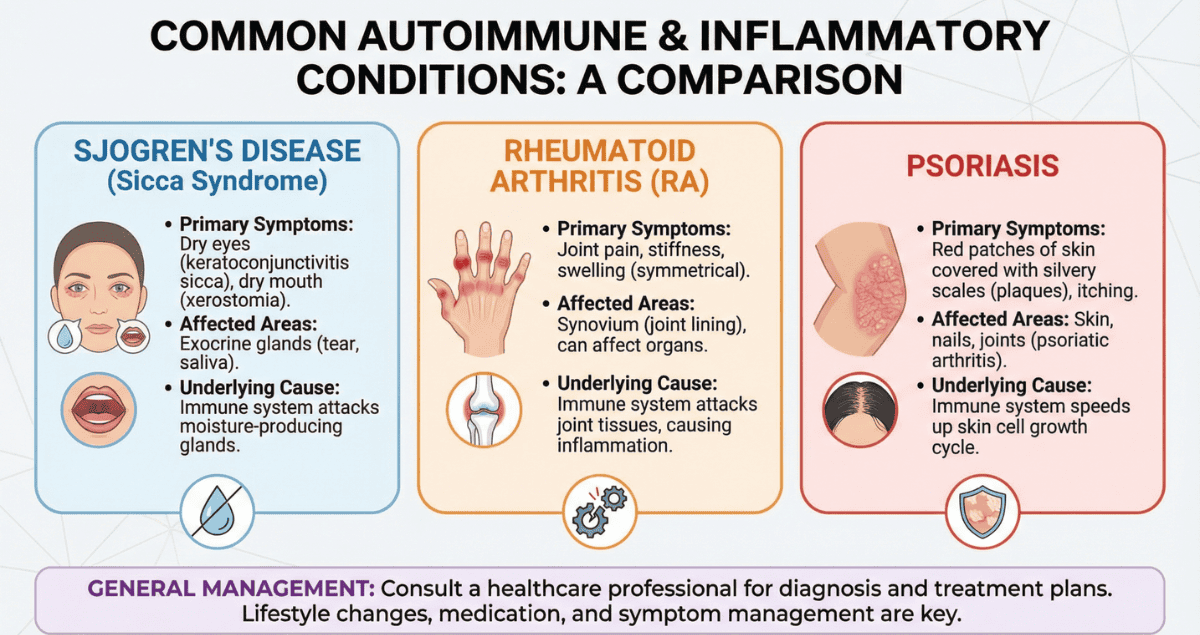
Beyond widely recognized autoimmune diseases like Hashimoto thyroiditis, celiac disease, and systemic lupus erythematosus, there are several other conditions that are frequently encountered in clinical practice and often require equally careful diagnostic evaluation. Among the most common in this next group are rheumatoid arthritis, psoriasis, and Sjögren syndrome.
Each of these diseases involves a distinct pattern of immune-mediated injury, affects different organ systems, and presents unique diagnostic challenges. While clinical features and laboratory tests often raise suspicion, biopsy can play a critical role in confirming the diagnosis, assessing severity, and excluding other conditions that may mimic autoimmune disease.
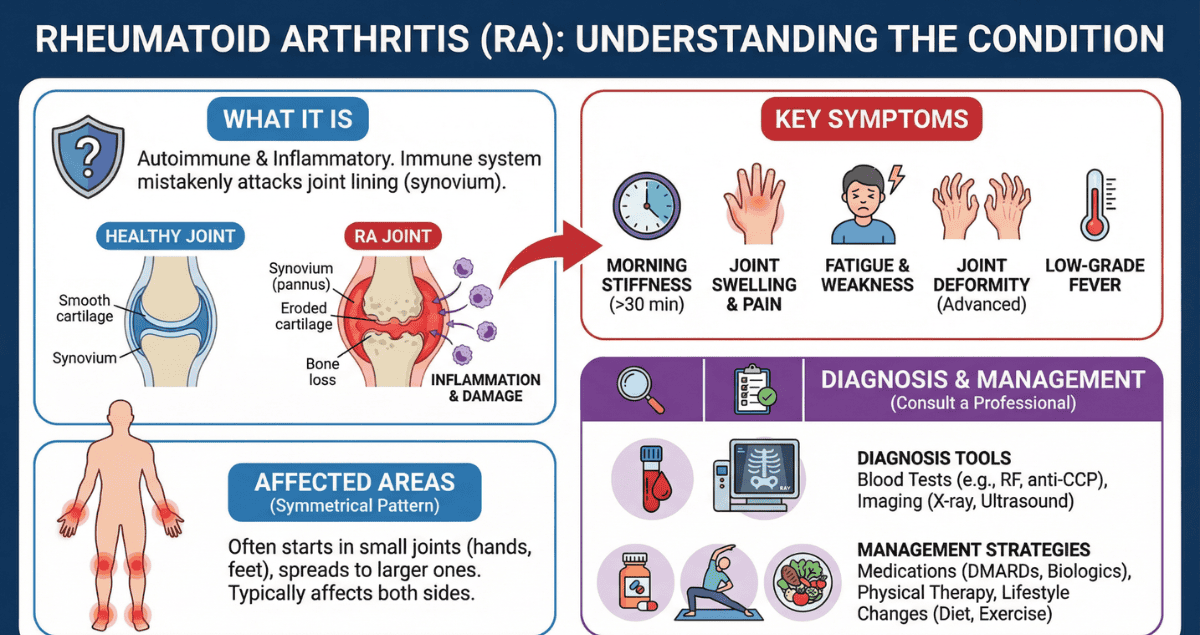
Rheumatoid Arthritis: When Joint Inflammation Becomes Systemic
Rheumatoid arthritis is a chronic autoimmune disease that primarily affects the joints, leading to pain, stiffness, and progressive damage. It is typically diagnosed based on clinical symptoms, imaging, and serologic markers such as rheumatoid factor and anti-CCP antibodies. However, biopsy can become important in certain scenarios.
Synovial biopsy, which involves sampling the lining of a joint, reveals characteristic histologic features of rheumatoid arthritis. These include synovial hyperplasia, dense infiltration by lymphocytes and plasma cells, and the formation of pannus, an aggressive tissue that erodes cartilage and bone.
Although biopsy is not routinely required for diagnosis, it can be particularly useful in atypical cases or when there is concern for infection or other inflammatory conditions. For example, distinguishing rheumatoid arthritis from infectious arthritis or other autoimmune arthritides may depend on microscopic evaluation.
Patients often wonder whether joint damage seen in rheumatoid arthritis is reversible. Biopsy findings help demonstrate that much of the damage is driven by chronic inflammation, underscoring the importance of early and accurate diagnosis to prevent long-term complications.
 Psoriasis: Skin Findings That Tell a Deeper Story
Psoriasis: Skin Findings That Tell a Deeper Story
Psoriasis is one of the most common autoimmune-mediated skin diseases, characterized by well-demarcated, scaly plaques. While it is often diagnosed clinically, skin biopsy can provide valuable confirmation, particularly in atypical presentations.
Histologically, psoriasis shows a distinctive pattern that includes epidermal hyperplasia, elongation of rete ridges, and parakeratosis, where nuclei are retained in the stratum corneum. Neutrophils may accumulate in the superficial layers, forming small collections known as Munro microabscesses.
One of the key roles of biopsy in psoriasis is distinguishing it from other skin conditions that may appear similar, such as eczema, fungal infections, or drug reactions. This distinction is important because treatment strategies differ significantly.
Patients frequently ask whether psoriasis is purely a skin condition. The answer is no. It is a systemic inflammatory disease that can also involve the joints, known as psoriatic arthritis. Biopsy helps confirm the cutaneous component, which may prompt further evaluation for systemic involvement.
Sjögren Syndrome: Subtle Findings with Significant Impact
Sjögren syndrome is an autoimmune disease that primarily affects exocrine glands, leading to dryness of the eyes and mouth. While symptoms may seem mild at first, the disease can have broader systemic effects and requires accurate diagnosis.
One of the most important diagnostic tools in Sjögren syndrome is minor salivary gland biopsy, typically taken from the inner lip. Histologic examination reveals focal lymphocytic sialadenitis, where clusters of lymphocytes surround and infiltrate salivary gland tissue.
The density and organization of these lymphocytic aggregates are critical for diagnosis. Pathologists often calculate a “focus score,” which quantifies the degree of inflammation and helps support the diagnosis when combined with clinical and serologic findings.
A common question is whether a biopsy is necessary if blood tests are positive. In many cases, biopsy provides confirmatory evidence, especially when symptoms are nonspecific or when other conditions need to be excluded. It can also help assess disease severity and guide management.
What Patients Should Know About Biopsy in Autoimmune Disease
Biopsy is often viewed as an invasive step, but it remains one of the most informative tools in diagnosing autoimmune conditions. It allows physicians to directly observe how the immune system is affecting specific tissues, offering insights that cannot be obtained through blood tests alone.
Patients frequently ask whether biopsy results are definitive. While biopsy provides strong evidence, it is typically interpreted alongside clinical findings and laboratory data. Autoimmune diseases are complex, and no single test tells the whole story.
Another common concern is whether biopsy can differentiate between autoimmune disease and other conditions. In many cases, it can. For example, synovial biopsy can help exclude infection in joint disease, skin biopsy can rule out mimickers of psoriasis, and salivary gland biopsy can distinguish Sjögren syndrome from other causes of gland dysfunction.
Why Clear Interpretation of Pathology Matters
Even when a biopsy is performed and a pathology report is generated, understanding the results is not always straightforward. Reports often contain technical terminology that can be difficult to interpret without specialized training.
This is where services like Honest Pathology become especially valuable. Honest Pathology focuses on translating complex biopsy findings into clear, understandable explanations. For patients navigating a new diagnosis or trying to make sense of their results, this added clarity can make a significant difference.
Rather than relying solely on brief or highly technical report summaries, patients can gain a deeper understanding of what their biopsy shows and how it relates to their symptoms and treatment options. This empowers more informed conversations with healthcare providers and helps reduce uncertainty.
The Expanding Role of Biopsy in Modern Autoimmune Care
As our understanding of autoimmune diseases continues to evolve, biopsy remains a cornerstone of diagnosis and disease assessment. It provides a level of detail that complements clinical evaluation and laboratory testing, helping to refine diagnoses and guide treatment decisions.
In diseases like rheumatoid arthritis, psoriasis, and Sjögren syndrome, biopsy may not always be the first step, but it often becomes essential when the diagnosis is unclear or when additional confirmation is needed. It also plays a role in identifying complications and monitoring disease progression.
Moving Forward with Confidence
Receiving a pathology report can feel overwhelming, especially when it includes unfamiliar terms or complex descriptions. Understanding the role of biopsy in autoimmune diseases is an important step in making sense of these findings.
For those seeking additional clarity, Honest Pathology offers a reliable and patient-focused resource. By providing clear explanations of biopsy results, it helps bridge the gap between medical terminology and real-world understanding.
In autoimmune disease, where early and accurate diagnosis can significantly impact outcomes, having access to clear, expert interpretation is not just helpful, it is essential.