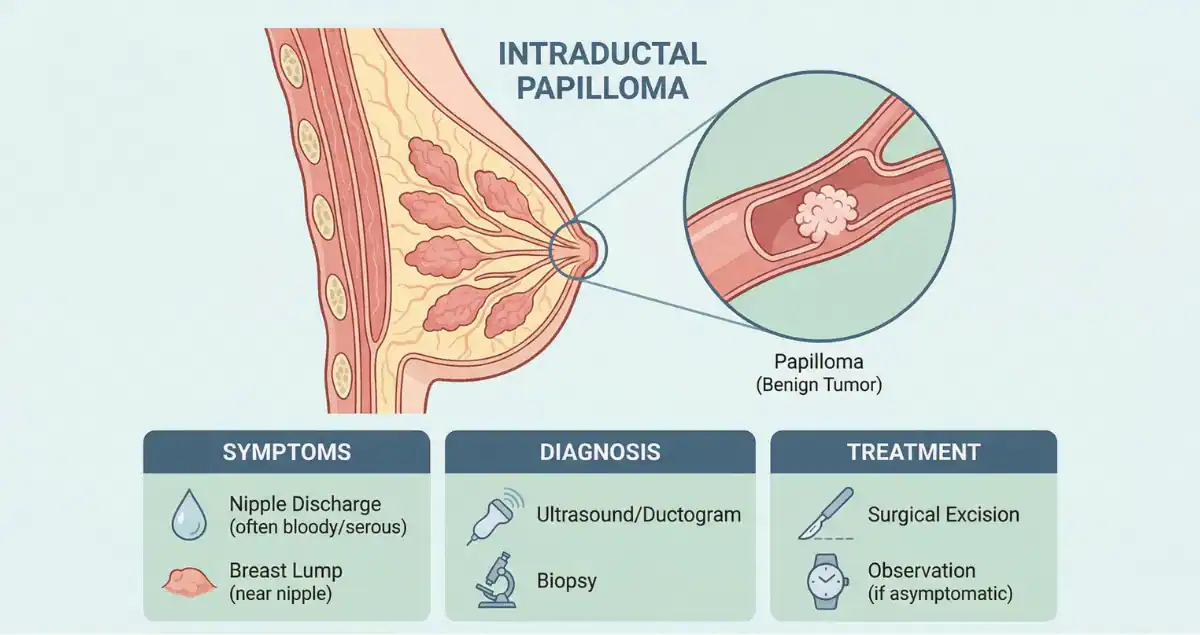
An intraductal papilloma is a benign tumor that arises within the milk ducts of the breast. Despite the word “tumor,” this lesion is non-cancerous and is composed of a small growth of epithelial and myoepithelial cells supported by a fibrovascular core. These growths typically develop inside a dilated duct and can occur either as a single lesion or as multiple papillomas.
Intraductal papillomas are most commonly found in women between the ages of 35 and 55, though they can occur outside this range. They are one of the more frequent benign breast lesions encountered in both imaging and pathology.
Common Symptoms and How They Present
Many intraductal papillomas present with nipple discharge, which may be clear or bloody. This is often what prompts further evaluation. Some patients may also notice a small lump near the nipple, especially when the papilloma is located in a central duct.
However, not all papillomas cause symptoms. Some are discovered incidentally on imaging studies such as mammography or ultrasound. This can raise understandable concern, especially when a biopsy is recommended.
A frequent question is whether nipple discharge always indicates something serious. While it should always be evaluated, intraductal papilloma is one of the most common benign causes of this symptom.
 What Does an Intraductal Papilloma Look Like Under the Microscope?
What Does an Intraductal Papilloma Look Like Under the Microscope?
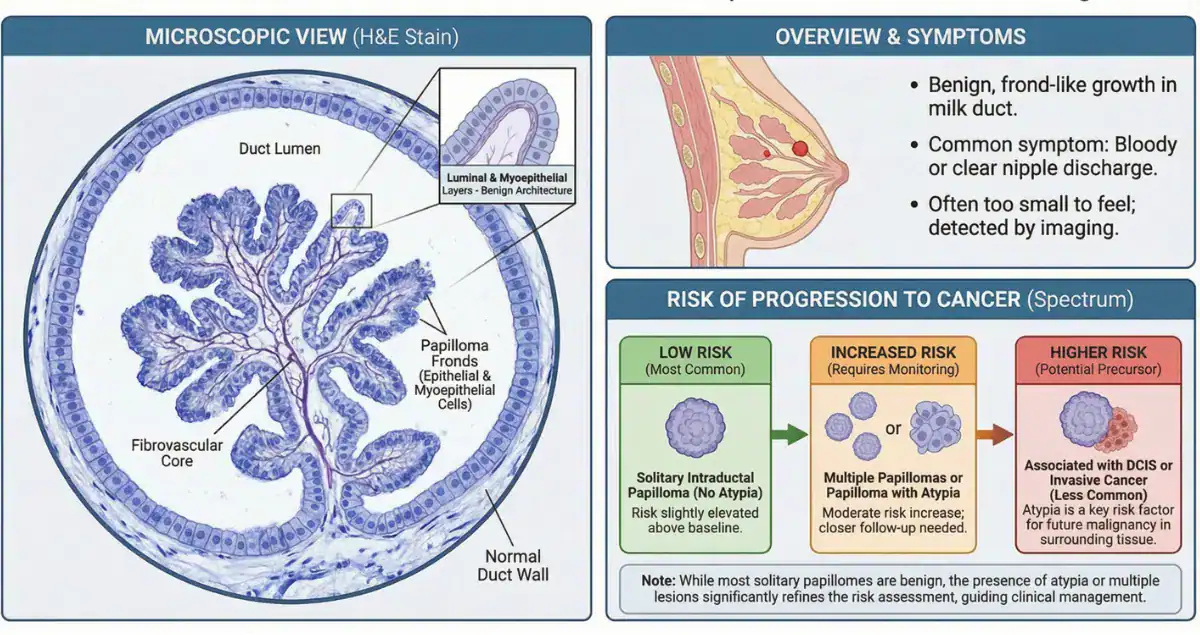
Histologically, intraductal papillomas have a distinctive appearance. They are characterized by branching fibrovascular cores lined by both epithelial and myoepithelial cells. The presence of this dual cell layer is a key feature that helps confirm the benign nature of the lesion.
The architecture often appears as finger-like projections extending into the ductal lumen. Pathologists carefully examine these structures to ensure there is no evidence of atypia or malignancy within the papilloma.
Sometimes, additional features such as usual ductal hyperplasia, apocrine metaplasia, or cystic change may be present. These findings fall within the spectrum of benign breast changes but can add complexity to the pathology report.
Can Intraductal Papillomas Become Cancer?
This is one of the most common and important concerns. The short answer is that most intraductal papillomas do not become cancer. However, the risk depends on specific features identified on biopsy.
A solitary papilloma without atypia carries a very low risk of progression to breast cancer. In many cases, once it is removed or adequately sampled, no further treatment beyond routine screening is needed.
However, if atypical cells are present within the papilloma, the situation changes. Atypical ductal hyperplasia or other atypical features can increase the risk of developing breast cancer over time. In these cases, surgical excision is often recommended to ensure that no more advanced lesion is present nearby.
Multiple papillomas, particularly those located in peripheral ducts, may also be associated with a slightly increased risk compared to a single central papilloma.
Why Is a Biopsy Necessary?
Imaging alone cannot always distinguish an intraductal papilloma from other breast lesions, including carcinoma. This is why biopsy is often recommended when a suspicious or unclear finding is identified.
A core needle biopsy allows pathologists to evaluate the tissue architecture and cellular features. This helps confirm the diagnosis and, importantly, assess whether any atypia or malignancy is present.
Patients often wonder whether a benign biopsy means no further action is needed. In some cases, particularly when imaging and pathology findings are perfectly aligned, observation may be appropriate. In other cases, surgical removal is advised to fully evaluate the lesion and eliminate any sampling uncertainty.
Do All Intraductal Papillomas Need to Be Removed?
Management depends on several factors, including whether atypia is present, how well the biopsy findings match the imaging results, and the patient’s overall risk profile.
For papillomas without atypia that are completely explained by imaging findings, some clinicians may recommend close monitoring rather than surgery. However, many still favor excision to ensure there is no hidden area of concern.
When atypia is identified, surgical excision is generally recommended. This is because a small biopsy sample may not capture the entire lesion, and more significant abnormalities could be present elsewhere in the tissue.
Understanding Your Pathology Report
Pathology reports for intraductal papilloma often include detailed descriptions that can feel difficult to interpret. Terms such as “fibrovascular core,” “myoepithelial layer,” or “associated atypia” carry important meaning but may not be immediately clear.
Patients frequently ask whether their specific findings change their cancer risk or follow-up plan. These are important questions, and the answers depend on the precise details of the report.
Getting Clarity with Honest Pathology
This is where a service like Honest Pathology can be especially helpful. Honest Pathology focuses on explaining biopsy results in clear, understandable language, helping patients make sense of complex findings.
For a condition like intraductal papilloma, where most cases are benign but some carry additional considerations, having a clear explanation can reduce anxiety and support better decision-making. Understanding whether atypia is present, what it means, and what steps to take next is essential.
Rather than navigating technical terminology alone, patients can gain confidence in their diagnosis and feel more prepared to discuss options with their healthcare provider.
What This Means for Your Long-Term Health
Intraductal papillomas are common and, in most cases, not dangerous. The key factor is whether atypia or other concerning features are present. With appropriate evaluation and follow-up, the vast majority of patients do very well.
Routine breast screening remains important, and any new symptoms should be evaluated promptly. Understanding your diagnosis is an important part of maintaining long-term breast health.
Moving Forward with Confidence
Hearing that you have a breast lesion, even a benign one can be stressful. Intraductal papilloma is a good example of a condition where careful evaluation provides reassurance in most cases while still identifying the minority of cases that need closer attention.
Biopsy plays a central role in this process, offering the detail needed to guide management decisions. For patients seeking clarity and peace of mind, Honest Pathology provides a trusted resource to better understand what their pathology report truly means.
With accurate information and the right support, it becomes much easier to move forward with confidence.