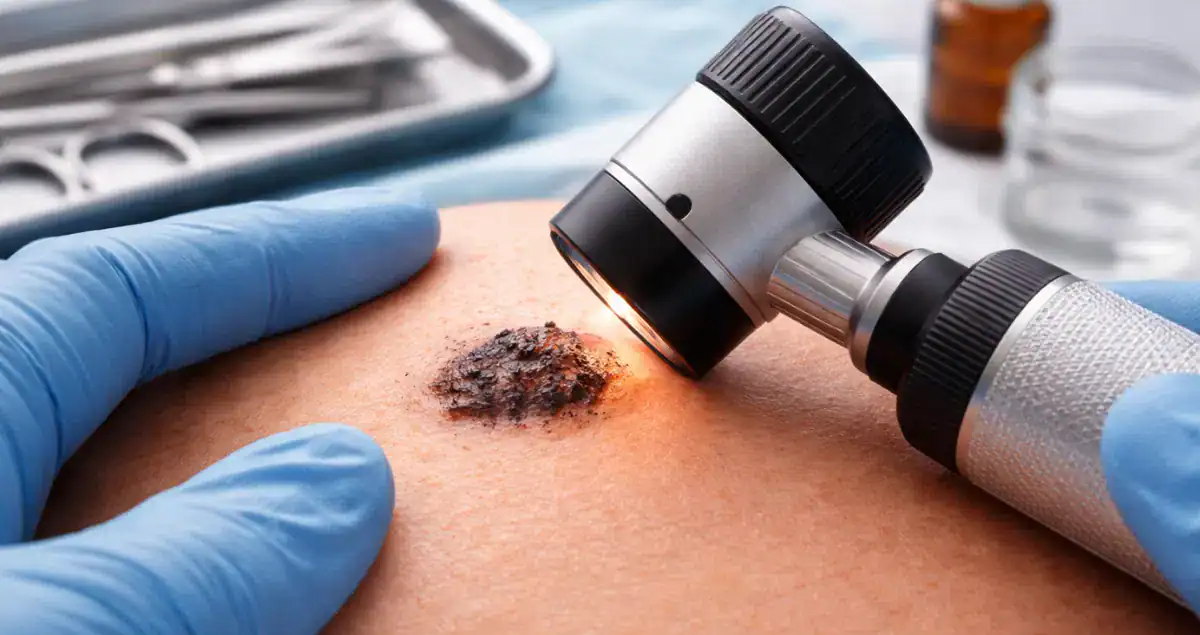
Melanoma in situ represents the earliest stage of melanoma, confined to the epidermis, the top layer of the skin. Because it has not penetrated deeper layers, it is considered highly treatable and carries an excellent prognosis. Despite its early stage, patients often have many questions about what melanoma in situ means, how it is managed, and how it differs from invasive melanoma.
At Honest Pathology, we help patients interpret pathology reports that include melanoma in situ, clarifying what the diagnosis means and how it fits into their overall care plan.
What Is Melanoma In Situ?
Melanoma in situ is a melanoma that remains confined to the epidermis. The term “in situ” is Latin for “in its original place,” indicating that the abnormal melanocytes have not invaded the dermis or deeper tissues.
Because it is limited to the surface layer, melanoma in situ does not have access to blood vessels or lymphatics, which are pathways for cancer to spread. This is why prognosis at this stage is excellent, with surgical excision typically being curative.
How Melanoma In Situ Is Diagnosed
Diagnosis begins with a skin biopsy. The type of biopsy—whether shave, punch, or excisional—depends on lesion size, location, and appearance. The tissue is then processed in the pathology laboratory, embedded in paraffin, sliced, stained, and examined under a microscope.
Pathologists look for abnormal melanocytes confined to the epidermis without evidence of invasion into the dermis. Features such as pagetoid spread, architectural disorder, and atypical nuclei help confirm the diagnosis. Accurate identification of melanoma in situ is crucial to guide appropriate surgical management.
Difference Between Melanoma In Situ and Invasive Melanoma
The key difference between melanoma in situ and invasive melanoma is depth of invasion. In situ lesions are limited to the epidermis, whereas invasive melanomas penetrate into the dermis and potentially beyond.
This distinction is important because invasive melanomas carry a higher risk of metastasis and require additional staging measures, such as assessment of Breslow depth, Clark level, and sometimes sentinel lymph node biopsy. Melanoma in situ, on the other hand, is effectively treated with complete excision and rarely requires further interventions.
Treatment of Melanoma In Situ
The primary treatment for melanoma in situ is surgical removal with appropriate margins. The recommended margin depends on the lesion’s size and location, typically ranging from 0.5 to 1 centimeter of normal-appearing skin around the lesion.
Mohs micrographic surgery may be considered in certain areas where tissue preservation is important, such as the face or fingers. This technique allows for complete removal while minimizing loss of healthy tissue.
Because melanoma in situ is confined to the epidermis, lymph node evaluation and systemic therapy are generally not indicated. Follow-up focuses on monitoring for recurrence or new lesions.
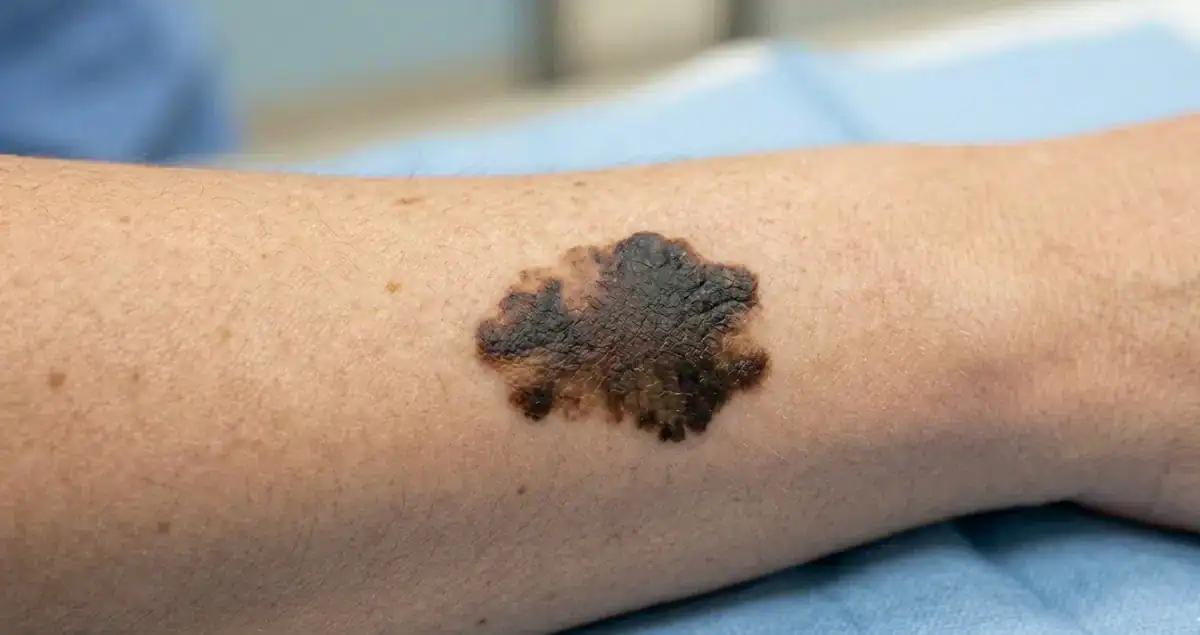 Prognosis for Melanoma In Situ
Prognosis for Melanoma In Situ
Melanoma in situ carries an excellent prognosis. When completely excised with negative margins, recurrence is uncommon. Long-term survival rates approach 100 percent.
Patients should remain vigilant for new or changing pigmented lesions, as individuals with melanoma in situ may have a higher lifetime risk of developing additional melanomas.
Recurrence and Follow-Up
Although melanoma in situ is highly treatable, careful follow-up is recommended. Follow-up typically includes regular skin exams by a dermatologist, with the frequency depending on individual risk factors, including family history, skin type, and sun exposure history.
Patients are also encouraged to perform self-examinations and report any new or changing lesions promptly. Early detection of any recurrence or new melanoma is key to maintaining excellent outcomes.
Common Questions About Melanoma In Situ
Patients often wonder if melanoma in situ will progress to invasive melanoma. While it has the potential to invade if left untreated, prompt and complete surgical removal prevents progression.
Another frequent concern is scarring. Surgical excision may leave a scar, the size of which depends on the location and extent of the lesion. Mohs surgery or other specialized techniques can minimize scarring in cosmetically sensitive areas.
Patients may also ask if melanoma in situ requires staging or imaging. Because the lesion is confined to the epidermis, additional staging tests are generally unnecessary unless there are unusual clinical features.
Risk Factors and Prevention
The development of melanoma in situ shares many risk factors with invasive melanoma. These include fair skin, history of sunburns, excessive ultraviolet exposure, multiple moles, family history of melanoma, and genetic predispositions.
Preventive strategies include daily sun protection, wearing protective clothing, avoiding tanning beds, and undergoing routine skin examinations. Early detection through vigilant monitoring is key to catching melanoma while it is still in situ.
How It Appears in Pathology Reports
A pathology report for melanoma in situ may read: “Melanoma in situ, epidermis only, margins negative, no evidence of invasion.”
This report indicates that the lesion is confined to the epidermis, has been completely excised, and shows no signs of deeper invasion. At Honest Pathology, we guide patients in interpreting these reports so they understand what the findings mean for their prognosis and follow-up care.
The Bottom Line
Melanoma in situ is an early-stage melanoma confined to the epidermis. It carries an excellent prognosis when completely excised and is rarely associated with metastasis. Understanding this diagnosis helps patients feel informed and reassured, while emphasizing the importance of follow-up and sun-protective behaviors.
By combining careful surgical management, regular dermatologic monitoring, and patient education, melanoma in situ is highly manageable. Honest Pathology focuses on helping patients understand their pathology reports and what each detail, including the in situ designation, means for their care and long-term outcomes.