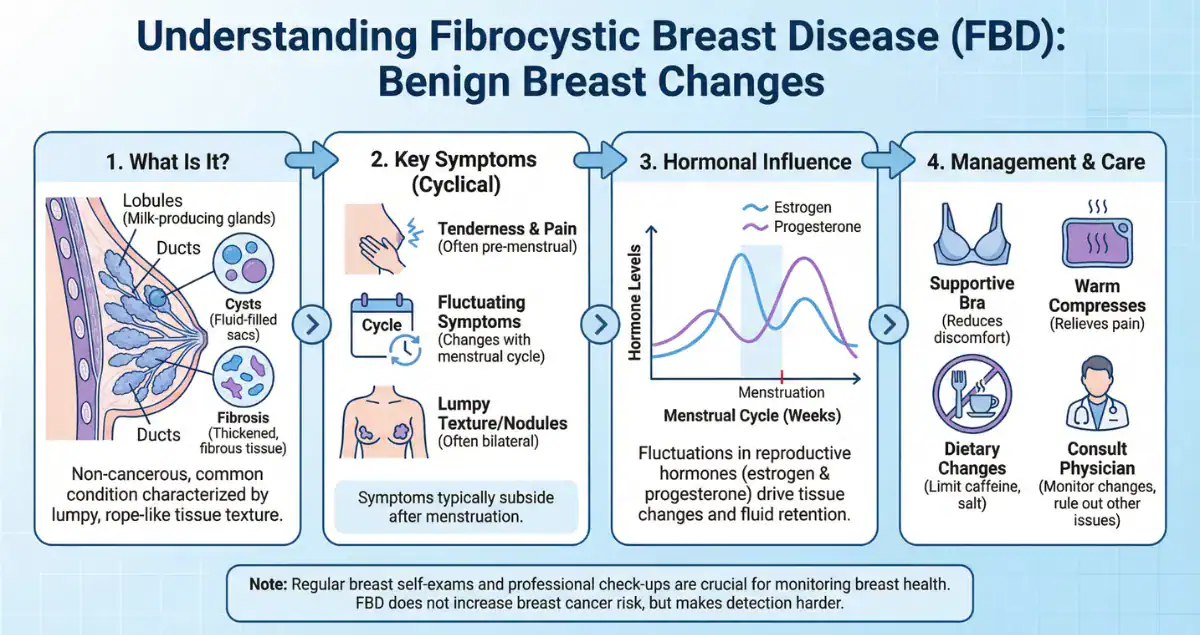
Fibrocystic breast disease, more accurately called fibrocystic breast changes, is one of the most common benign conditions affecting the breast. Despite the word “disease,” it is not a true disease but rather a spectrum of normal, non-cancerous changes that occur in response to hormonal fluctuations, particularly estrogen and progesterone.
Many women experience these changes at some point in their lives, especially during reproductive years. The condition often presents as breast lumpiness, tenderness, or cyclical discomfort that worsens before menstruation. While these symptoms can be concerning, fibrocystic changes are extremely common and, in most cases, not dangerous.
Why Do These Changes Happen?
Fibrocystic changes are driven largely by hormonal influence on breast tissue. The breast is highly responsive to hormonal cycles, and over time, repeated stimulation can lead to structural changes within the tissue.
This includes the development of cysts, areas of fibrosis, and proliferation of glandular components. These changes can make the breast feel nodular or dense, which is why many patients notice lumps or areas of thickening.
A common question is whether these lumps are permanent. Some may fluctuate or even resolve over time, particularly with changes in hormone levels, while others may persist. This variability is part of what makes the condition feel unpredictable.
What Does Fibrocystic Change Look Like Under the Microscope?
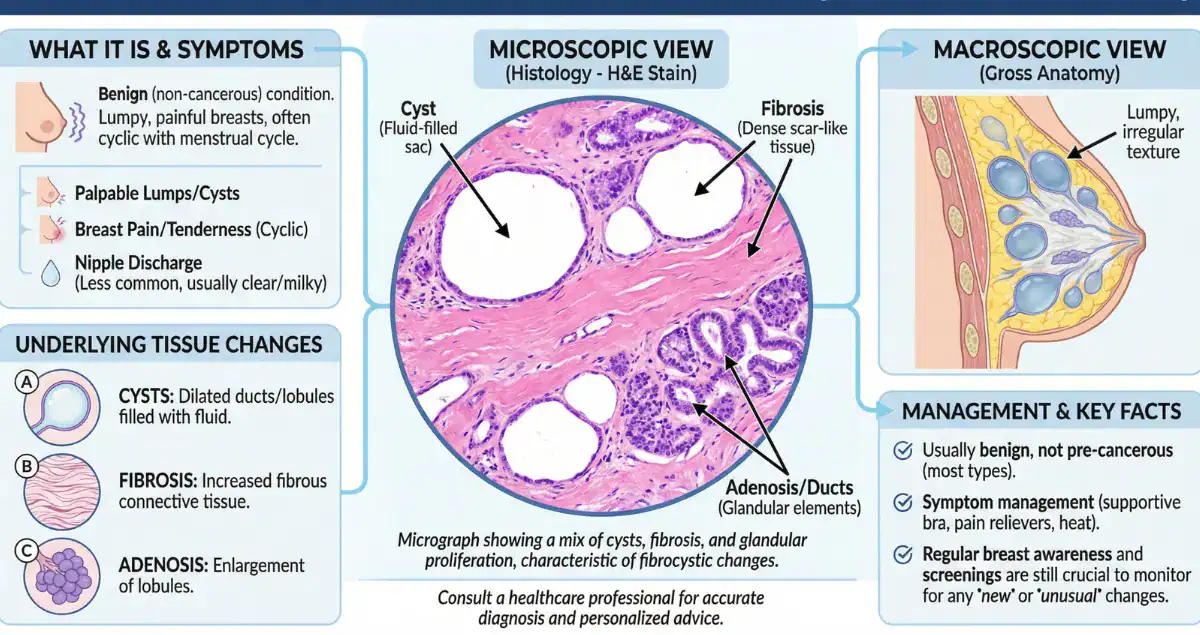
When a biopsy is performed, fibrocystic changes reveal a range of characteristic histologic findings. One of the most common is cyst formation, where dilated ducts are filled with fluid. These cysts may be lined by flattened or apocrine-type epithelial cells, which often have abundant, granular cytoplasm.
Fibrosis is another key feature. The stroma surrounding ducts and lobules becomes dense and collagenized, contributing to the firm texture that patients may feel during self-examination or clinical evaluation.
Additional findings can include adenosis, where there is an increased number of glandular structures, and usual ductal hyperplasia, which involves a proliferation of epithelial cells within the ducts. Importantly, these changes are benign, though some patterns of proliferation may slightly increase long-term breast cancer risk.
These microscopic features help pathologists distinguish fibrocystic changes from more concerning lesions, ensuring that benign findings are not overinterpreted as malignancy.
 Does Fibrocystic Breast Change Increase Cancer Risk?
Does Fibrocystic Breast Change Increase Cancer Risk?
This is one of the most frequently asked and important questions. The answer depends on the specific histologic features present.
Simple fibrocystic changes, such as cysts and fibrosis without significant epithelial proliferation, do not increase breast cancer risk. However, certain proliferative changes, particularly those with atypia, may be associated with a higher risk over time.
This is why biopsy and accurate pathology interpretation are so important. The exact wording of a pathology report can provide critical information about risk and guide appropriate follow-up.
When Is a Biopsy Needed?
Not all fibrocystic changes require biopsy. Many cases are diagnosed based on clinical examination and imaging, such as mammography or ultrasound. However, biopsy is recommended when there are features that cannot be confidently classified as benign.
This may include a new or persistent lump, imaging findings that are unclear, or changes that do not follow the typical pattern of fibrocystic disease. The goal of biopsy is to rule out malignancy and provide a definitive diagnosis.
Patients often ask whether biopsy is painful or risky. While any procedure carries some risk, breast biopsies are generally safe and minimally invasive, and the information they provide is invaluable.
Why Do Fibrocystic Changes Hurt?
Breast pain associated with fibrocystic changes is usually cyclical and linked to hormonal fluctuations. As hormone levels rise and fall במהלך the menstrual cycle, breast tissue can become swollen and more sensitive.
Cysts may enlarge during this time, and the surrounding fibrotic tissue can contribute to a feeling of tightness or discomfort. This pain is typically not a sign of cancer, but it can still be distressing.
Understanding the underlying cause of the pain often helps reduce anxiety, especially when serious conditions have been ruled out.
Can Fibrocystic Changes Go Away?
Another common concern is whether fibrocystic changes are permanent. In many cases, symptoms improve over time, particularly after menopause when hormonal stimulation decreases.
However, some structural changes within the breast may persist. The key point is that these changes are benign and manageable, even if they do not completely disappear.
Lifestyle modifications, supportive measures, and in some cases medical management can help alleviate symptoms.
Why Pathology Reports Can Feel Confusing
Even when a biopsy confirms fibrocystic changes, the language in a pathology report can feel overwhelming. Terms like “apocrine metaplasia,” “stromal fibrosis,” or “ductal hyperplasia” are not always intuitive, yet they carry important meaning.
Patients often leave with more questions than answers, wondering what these findings mean for their health and future risk. This is a common and understandable experience.
Getting Clear Answers with Honest Pathology
This is where services like Honest Pathology can make a meaningful difference. Honest Pathology focuses on helping patients truly understand their pathology reports by translating complex medical language into clear, accessible explanations.
Instead of trying to interpret unfamiliar terminology alone, patients can gain insight into what their biopsy shows, what is benign, and whether any findings require follow-up. This added clarity can reduce anxiety and support more confident decision-making.
For something as common and often misunderstood,as fibrocystic breast changes, having a trusted resource to explain the details can be incredibly valuable.
Moving Forward with Confidence
Fibrocystic breast changes are a normal and very common part of breast health for many women. While the symptoms and findings can feel concerning, the vast majority of cases are benign and manageable.
Understanding what these changes mean, both clinically and microscopically, helps put pathology reports into perspective. It also highlights the importance of accurate diagnosis and clear communication.
For those seeking reassurance or a deeper understanding of their results, . In a situation where uncertainty is common, having clear answers can make all the difference.