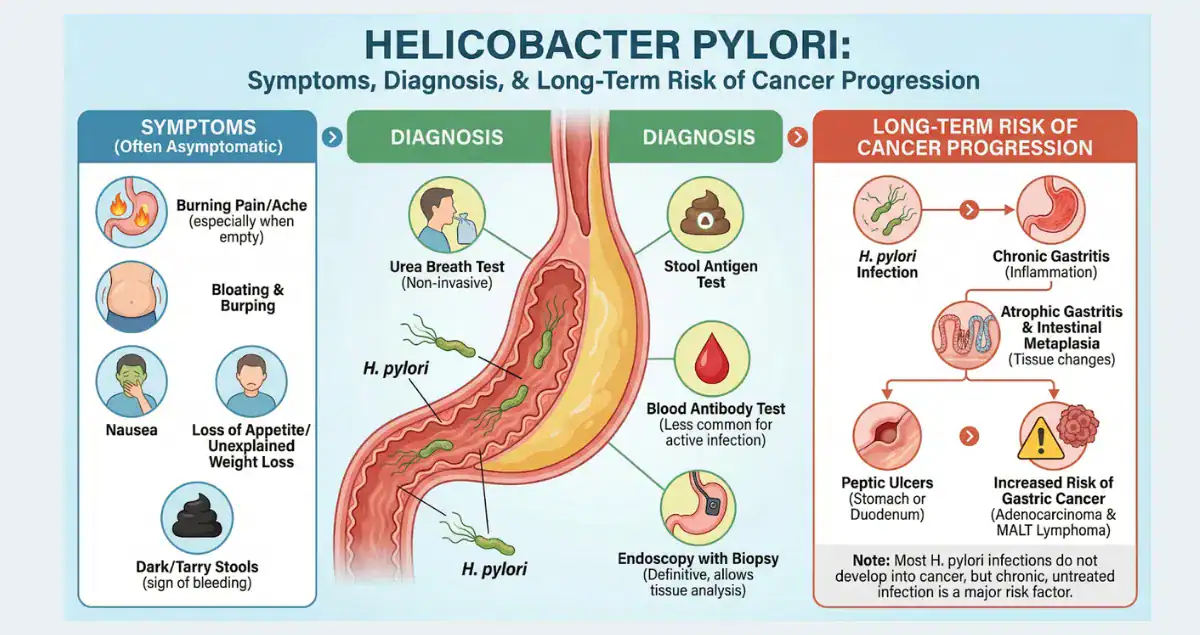
Gastritis is one of the most frequent diagnoses made after upper endoscopy, yet many patients feel uncertain when they receive their pathology report. The condition involves inflammation of the stomach lining and exists in several distinct forms, each carrying different risks of progressing to gastric cancer over time. While the absolute risk remains low for most people, certain chronic types can slowly advance through a series of changes that increase the chance of adenocarcinoma.
Pathology evaluation of stomach biopsies provides the clearest picture of the gastritis type and any precancerous features such as atrophy or intestinal metaplasia. Honest Pathology delivers expert pathology consultations that turn these detailed reports into plain-language explanations, empowering patients to understand their personal risk and make informed decisions about surveillance and lifestyle changes.
What Is Gastritis and Why Cancer Risk Varies by Type
Gastritis refers to inflammation of the gastric mucosa. It can be acute or chronic, infectious or chemical, and the long-term cancer risk depends heavily on the specific pattern seen under the microscope. Most forms of gastritis cause no progression to cancer, but a subset involving persistent damage can follow the Correa cascade: chronic gastritis → atrophic gastritis → intestinal metaplasia → dysplasia → adenocarcinoma. Honest Pathology consultations help patients see exactly where their biopsy fits on this pathway, providing clarity that reduces anxiety and supports proactive care.
Acute Gastritis: Low Long-Term Risk and Quick Resolution
Acute gastritis develops rapidly from triggers such as heavy alcohol intake, NSAID medications, stress, or infections. Biopsy shows surface erosions and neutrophil-rich inflammation without deep structural damage. The condition usually resolves within days to weeks once the cause is removed, and the 10-year risk of progressing to stomach cancer is essentially zero in uncomplicated cases. Patients often worry that one episode will lead to lasting problems, but pathology typically confirms only temporary changes with excellent recovery potential. Honest Pathology explains these reassuring findings clearly, helping patients focus on prevention rather than fear.
Chronic Non-Atrophic Gastritis: Common but Very Low Cancer Risk
Chronic non-atrophic gastritis is the most frequently reported type and features increased lymphocytes and plasma cells without significant gland loss. Helicobacter pylori infection is the leading cause worldwide. On biopsy, inflammation remains superficial, and the normal glandular architecture is preserved. The 10-year risk of developing gastric cancer in uncomplicated chronic non-atrophic gastritis is very low, generally estimated at less than 1%. Many patients remain stable for decades, especially after successful H. pylori eradication. Honest Pathology reviews the biopsy to confirm the absence of atrophy or metaplasia, giving patients confidence that their condition carries minimal long-term cancer concern.
Atrophic Gastritis: Noticeably Higher Risk That Depends on Severity
Atrophic gastritis involves loss of normal gastric glands and is classified as mild, moderate, or severe based on how much mucosa is affected. When driven by long-standing H. pylori, the 10-year risk of gastric cancer ranges from approximately 2% to 6%, depending on the extent of atrophy. Autoimmune gastritis, which destroys acid-producing cells, carries a similar or slightly higher risk, particularly when severe atrophy is present. Biopsy reveals thinned mucosa with fibrosis and reduced glands.
Patients often ask whether atrophic gastritis inevitably leads to cancer. While progression is possible, many cases remain stable for years with proper management and surveillance. Honest Pathology pinpoints the precise degree of atrophy and any accompanying changes, allowing patients to understand their individualized risk and the rationale for recommended follow-up endoscopy intervals.
Intestinal Metaplasia: A Key Precancerous Change with Quantifiable Risk
Intestinal metaplasia occurs when stomach lining cells are replaced by intestinal-type cells, visible on biopsy with special stains that highlight goblet cells. This finding marks an important step in the progression pathway. The 10-year risk of developing gastric cancer in patients with intestinal metaplasia is estimated at 5% to 10% overall, but it can be lower (around 3-5%) in limited cases or higher (up to 15% or more) when the metaplasia is extensive, incomplete, or located in the body of the stomach. H. pylori eradication can sometimes lead to partial regression and lower future risk. Patients frequently worry after seeing this term on their report. Honest Pathology explains the extent and type of metaplasia seen on their specific slides, helping them weigh the benefits of regular surveillance against quality-of-life considerations.
Autoimmune Gastritis and Its Distinct Cancer Risks
Autoimmune gastritis primarily affects the upper stomach and leads to profound atrophy and vitamin B12 deficiency. Biopsy shows dense lymphocytic infiltration and loss of parietal cells, often with enterochromaffin-like cell hyperplasia. The 10-year risk of gastric adenocarcinoma is approximately 5% to 8%, while the risk of type 1 gastric neuroendocrine tumors is also elevated, sometimes reaching 5% to 10% over 10 years in long-standing cases. Because symptoms may relate more to anemia than stomach discomfort, diagnosis can be delayed. Honest Pathology highlights these characteristic features, enabling patients to coordinate comprehensive care that includes both cancer surveillance and nutritional management.
Chemical/Reactive Gastritis: Minimal Cancer Risk
Chemical or reactive gastritis results from bile reflux, long-term NSAID use, or alcohol and shows foveolar hyperplasia with little inflammation on biopsy. Because it rarely progresses to atrophy or metaplasia, the 10-year risk of stomach cancer is very low, typically under 1%. Symptoms often improve when the offending agent is reduced or eliminated. Honest Pathology quickly identifies this pattern, reassuring patients that their gastritis is unlikely to carry significant long-term cancer risk and focusing discussion on practical symptom relief.
The Correa Cascade: How Gastritis Can Progress to Cancer Over Time
The pathway from gastritis to cancer usually follows a slow, stepwise process. Chronic inflammation can lead to glandular atrophy, then intestinal metaplasia, low-grade dysplasia, high-grade dysplasia, and finally invasive cancer. Each step increases risk, but the majority of patients never advance beyond early stages. H. pylori eradication can interrupt this cascade at multiple points and substantially reduce cancer incidence. Progression timelines vary from decades in some individuals to faster advancement in others with additional risk factors. Honest Pathology provides precise grading of any precancerous changes, helping patients understand their position on the cascade and the value of timely intervention.
Factors That Influence Progression Risk
Several factors modify the chance that gastritis will advance. Persistent H. pylori infection, smoking, high-salt diet, family history of gastric cancer, and extensive atrophy or metaplasia on biopsy increase risk. Conversely, successful eradication of H. pylori, antioxidant-rich diets, smoking cessation, and regular surveillance can lower progression rates significantly. Age and male sex also correlate with slightly higher risk. Honest Pathology integrates these clinical factors with biopsy findings to give patients a more personalized view of their 10-year risk and practical steps they can take to improve their outlook.
How Honest Pathology Empowers Patients with Gastritis Diagnoses
A pathology report mentioning chronic gastritis, atrophy, intestinal metaplasia, or dysplasia can feel overwhelming due to medical terminology and uncertain implications. Honest Pathology offers focused consultations that explain every element of the report in clear terms: the exact type of gastritis, the presence and degree of atrophy or metaplasia, and what those findings mean for 10-year cancer risk. Patients gain the knowledge needed to have productive conversations with their gastroenterologist about surveillance intervals, lifestyle modifications, and when further testing might be warranted. This level of understanding transforms a potentially frightening diagnosis into an opportunity for informed, confident decision-making.
Stomach cancer is a serious but largely preventable outcome of specific chronic gastritis patterns. By distinguishing between low-risk and higher-risk forms through expert pathology review, patients can take targeted actions that significantly improve their long-term prognosis. Honest Pathology exists to make this process accessible, turning complex biopsy results into practical guidance that supports better health outcomes and greater peace of mind at every stage of gastritis.