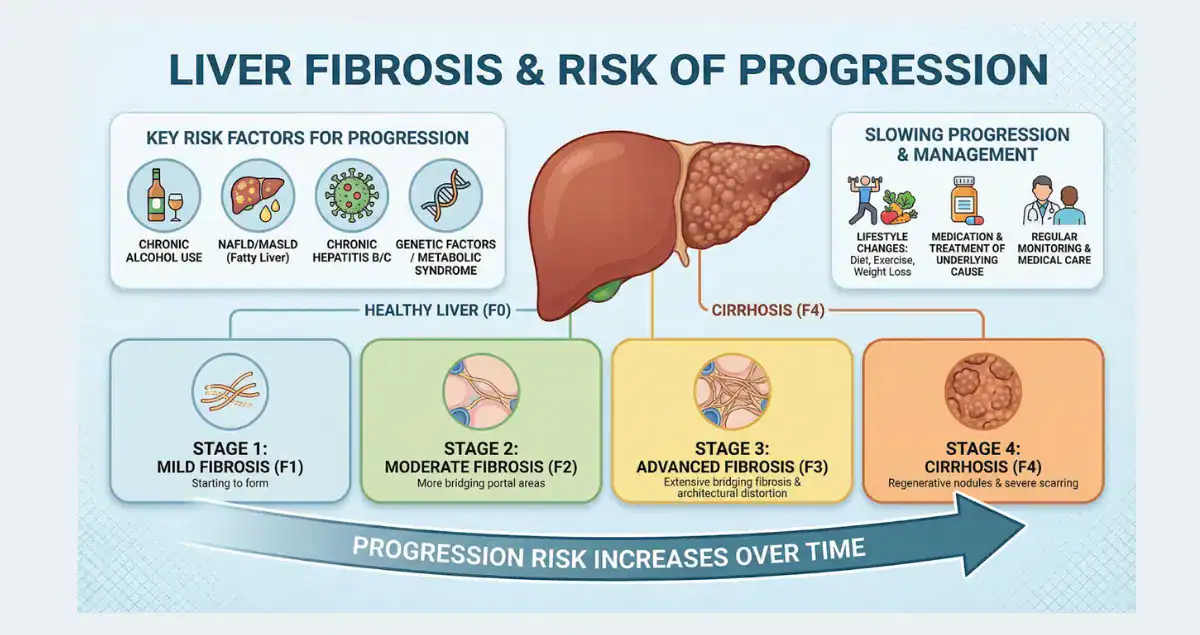
Liver fibrosis develops gradually as the liver tries to repair ongoing damage from causes such as viral hepatitis, metabolic dysfunction-associated steatotic liver disease, alcohol use, or autoimmune conditions. Many patients first learn about possible fibrosis after seeing elevated ALT or AST on routine blood tests or after imaging raises concerns. The stages of fibrosis range from mild, often reversible scarring to advanced changes that can progress toward cirrhosis. Accurate assessment through a liver biopsy provides the clearest view of how much scar tissue has formed and whether active inflammation is present.
Pathology reports frequently use scoring systems like METAVIR or Ishak to describe the stage, and they may also include the term MASH (Metabolic Dysfunction-Associated Steatohepatitis), which indicates a specific pattern of inflammation and fat accumulation that drives fibrosis in many people today. Honest Pathology offers expert pathology consultations that translate these detailed reports, including mentions of MASH, fibrosis stage, and enzyme trends, into plain, understandable language, empowering patients to grasp their exact situation and take confident steps in their care.
What Is Liver Fibrosis and Why Staging Through Pathology Matters
Liver fibrosis occurs when repeated injury causes the liver to deposit excess collagen and other proteins as scar tissue. A healthy liver is soft and efficient, but scarring makes it stiffer and can eventually interfere with blood flow and normal function. Staging evaluates how far the scarring has advanced and whether the normal liver architecture is still preserved. Pathologists examine biopsy samples microscopically, looking at the amount and pattern of scar tissue as well as any ongoing inflammation or fat buildup.
Common scoring systems rate fibrosis from none (F0) to cirrhosis (F4). When the report mentions MASH, it means the biopsy shows not only fibrosis but also steatosis (fat in liver cells) combined with inflammation and hepatocyte injury, a combination that accelerates scarring in metabolic liver disease. Understanding whether MASH is present alongside the fibrosis stage helps guide treatment because MASH-related fibrosis often responds well to weight loss and metabolic improvements. Honest Pathology consultations review these combined findings so patients clearly see how MASH and fibrosis interact in their specific case.
ALT and AST Blood Tests: Their Role Alongside Pathology Findings
ALT (alanine aminotransferase) and AST (aspartate aminotransferase) are enzymes released when liver cells are damaged. ALT tends to be more liver-specific, while AST can rise from other tissues as well. Elevated levels often prompt further investigation, including biopsy, because they can signal active injury that may contribute to fibrosis. However, ALT and AST do not directly measure scar tissue. Many patients with moderate or advanced fibrosis have normal or only mildly elevated enzymes, especially once active inflammation quiets. In cases where MASH is present on biopsy, ALT and AST are frequently elevated due to ongoing hepatocyte ballooning and inflammation.
The AST to ALT ratio can sometimes hint at the underlying cause, higher AST may point toward alcohol-related injury, while ALT often predominates in MASH or viral hepatitis. These blood tests provide useful information about current liver stress, but the biopsy gives the definitive picture of fibrosis stage and whether MASH is contributing. Honest Pathology helps patients connect their ALT and AST trends with the microscopic findings, explaining why enzyme levels may or may not match the reported fibrosis stage.
Early-Stage Liver Fibrosis: Mild Changes Often Seen with MASH
In early fibrosis, scar tissue is usually limited to the portal areas with thin collagen strands and little distortion of normal liver structure. Pathologists may describe mild portal fibrosis alongside steatosis and mild inflammation when MASH is present. ALT and AST can be mildly elevated due to the inflammatory component of MASH, but they are sometimes normal. At this stage, many people have no noticeable symptoms.
The prognosis is excellent because early fibrosis, especially when driven by MASH, frequently improves or even reverses with lifestyle changes such as sustained weight loss, better diet, and increased physical activity. Controlling MASH early can halt or reduce the scarring process before it advances. Honest Pathology consultations clarify whether the biopsy shows only mild fibrosis with MASH features and emphasize the strong potential for improvement when patients address metabolic factors.
Moderate Liver Fibrosis: Bridging Scars and Active MASH
Moderate fibrosis shows short fibrous bridges connecting portal tracts, with increasing distortion of the liver architecture but without full regenerative nodules. When MASH is noted on the pathology report, pathologists often describe steatosis, lobular inflammation, and hepatocyte ballooning in addition to the bridging fibrosis. ALT and AST are commonly elevated in this setting because of the active inflammatory process. Patients may start to feel more fatigue or mild abdominal discomfort.
The outlook remains encouraging with prompt intervention. Treating the metabolic drivers of MASH through weight reduction, diabetes management, and lifestyle modification can slow or stop progression and sometimes lead to partial regression of fibrosis. Honest Pathology explains the degree of bridging fibrosis and the contribution of MASH, helping patients understand why addressing metabolic health is central to improving their prognosis at this stage.
Advanced Liver Fibrosis: Significant Scarring with or without MASH
In advanced fibrosis, thick bridging septa extensively connect different areas of the liver, causing marked architectural distortion. MASH may still be present or may have quieted, leaving predominantly fibrotic changes. Biopsy reveals thick collagen bands with significant remodeling. ALT and AST levels vary, they may remain elevated if MASH activity continues or become nearer to normal as inflammation decreases. Symptoms such as itching, easy bruising, or mild swelling can appear.
While complete reversal is more challenging, stabilization and some improvement are still possible with aggressive management of metabolic factors and the underlying cause. Regular monitoring for complications becomes important. Honest Pathology provides a detailed breakdown of the biopsy, highlighting the extent of advanced fibrosis and whether residual MASH features are contributing to ongoing risk, so patients can plan appropriate surveillance and therapy.
Cirrhosis: The Most Advanced Stage of Fibrosis
Cirrhosis develops when dense scar tissue surrounds regenerative nodules and fully disrupts normal liver architecture. Pathology reports describe nodular regeneration encircled by broad fibrous bands. MASH may coexist in earlier phases of cirrhosis but often becomes less prominent as the disease advances. ALT and AST are frequently normal or only mildly abnormal in stable cirrhosis.
In compensated cirrhosis, many patients live well for years with good medical care. Decompensated cirrhosis, with fluid buildup, bleeding, or confusion, involves higher risks and may require transplant evaluation. Prognosis improves substantially when the original cause, including any metabolic components from prior MASH, is well controlled and complications are prevented. Honest Pathology consultations confirm the stage of cirrhosis, note any remaining MASH activity or other important features, and help patients understand their position on the spectrum so they can work effectively with their medical team.
How Honest Pathology Empowers Patients Through Clear Report Interpretation
Pathology reports that mention fibrosis stage, MASH, inflammation, or steatosis can feel technical and confusing. Honest Pathology specializes in patient-focused consultations that explain these findings in straightforward terms. Patients learn exactly what their biopsy shows regarding fibrosis stage, whether MASH is contributing, how the ALT and AST results fit into the picture, and what the combined findings suggest for prognosis and management. This clarity allows more productive conversations with hepatologists and supports confident decisions about lifestyle changes, medications, and follow-up care. By making complex pathology accessible, Honest Pathology helps turn a potentially worrying diagnosis into an opportunity for informed action at any stage of liver fibrosis.
Liver fibrosis exists on a continuum, from early mild changes that often respond well to intervention to advanced cirrhosis that requires careful long-term management. ALT and AST provide clues about active injury, while biopsy reveals the true pattern of scarring and the role of MASH when present. Through expert pathology consultations, Honest Pathology ensures patients receive clear, personalized explanations of their reports. This understanding equips individuals to address modifiable factors, monitor progress effectively, and approach their liver health with knowledge and optimism.