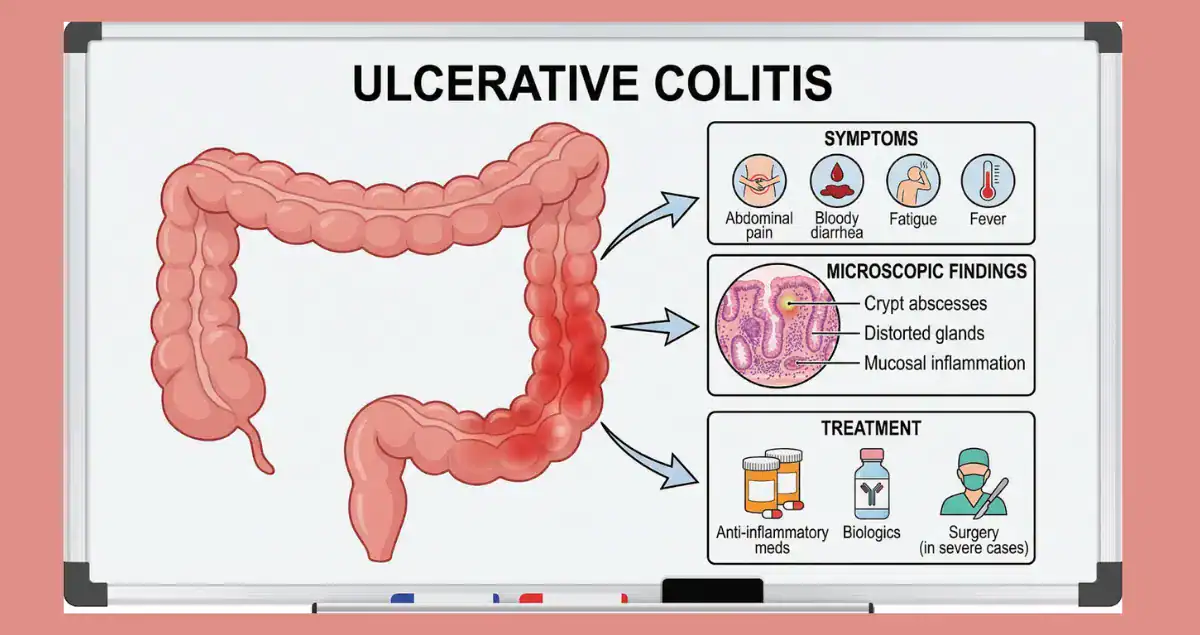
The gastrointestinal tract commonly shows reactive changes because it faces constant exposure to acid, bacteria, medications, and mechanical stress. In esophageal biopsies, reactive squamous epithelial changes are most often linked to gastroesophageal reflux disease (GERD). The lining thickens with basal cell hyperplasia, elongated papillae, and scattered inflammatory cells as the tissue attempts to protect itself from acid damage. Patients may experience heartburn, regurgitation, or swallowing discomfort. When reactive changes appear at the gastroesophageal junction, they can overlap with carditis and occasionally progress toward intestinal metaplasia if reflux remains untreated. Stomach biopsies frequently reveal reactive gastropathy or chemical gastritis, characterized by foveolar hyperplasia, smooth muscle proliferation in the lamina propria, and minimal inflammation.
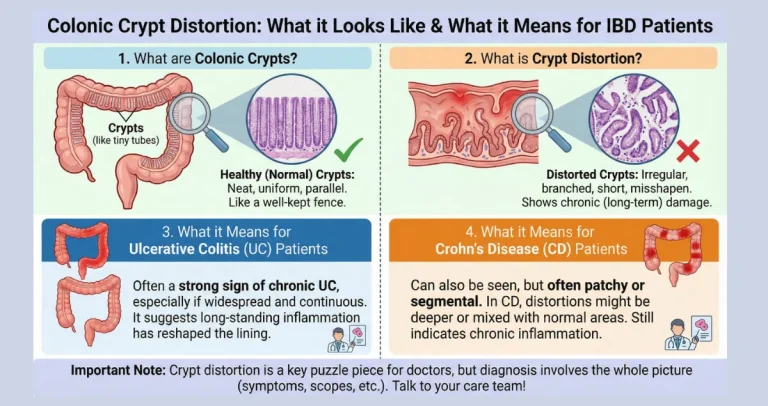
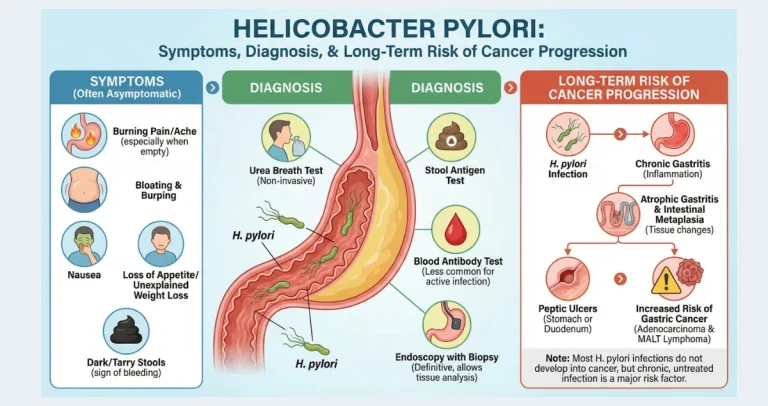
Common triggers include nonsteroidal anti-inflammatory drugs (NSAIDs), alcohol, bile reflux, or stress-related mucosal injury. Unlike H. pylori-associated gastritis, reactive gastropathy shows little lymphocytic infiltrate but prominent regenerative changes. In the colon and small intestine, reactive epithelial changes can appear in the setting of inflammatory bowel disease, infections, or ischemia. Crypts may show regenerative atypia with enlarged nuclei during active healing phases, which can occasionally raise concern for dysplasia until context is clarified. Ischemic colitis often produces reactive surface epithelial changes alongside hyalinized lamina propria.
Patients searching “reactive changes GI biopsy meaning” commonly wonder whether this finding requires immediate treatment or indicates permanent damage. Most reactive changes are reversible once the offending agent is removed—acid suppression for reflux, stopping NSAIDs for gastropathy, or treating underlying infection or inflammation. Expert pathology consultation helps distinguish pure reactive patterns from those bordering on dysplasia, giving patients confidence in the recommended management plan.
Reactive Changes in Breast Biopsies: Common Causes and Reassurance
Breast biopsies frequently demonstrate reactive changes following injury, prior procedures, or benign proliferative conditions. Fat necrosis is a classic example, where trauma, surgery, or radiation leads to damaged fat cells that elicit a reactive response with foamy macrophages, fibroblasts, and mild nuclear enlargement in surrounding tissue. This can create a firm lump or suspicious appearance on mammography, prompting biopsy. Post-biopsy reactive changes themselves are common, showing granulation tissue, reactive fibroblasts, and mild atypia along the needle tract that typically resolves over time.
Radial scars or complex sclerosing lesions often display reactive epithelial changes in entrapped ducts, which pathologists carefully evaluate to exclude associated atypia or carcinoma. Fibrocystic changes with usual ductal hyperplasia can include reactive nuclear features as the breast tissue responds to hormonal fluctuations or minor injury. Patients often worry whether reactive changes on breast biopsy mean higher cancer risk or hidden malignancy. Isolated reactive changes are almost always benign and do not significantly elevate future risk on their own.
However, when they occur within certain proliferative lesions, closer evaluation or follow-up imaging may be advised. Management is usually conservative, observation, pain control, or addressing any underlying cause such as stopping hormonal therapies that exacerbate fibrocystic changes. Pathology consultation provides reassurance by explaining the specific context of the reactive findings and clarifying whether additional testing or surveillance is warranted, helping patients discuss next steps knowledgeably with their breast care team.
Reactive Changes in Lung Biopsies: Response to Injury and Inflammation
Lung tissue is highly reactive to inhaled irritants, infections, and mechanical or chemical injury, making reactive changes a frequent biopsy finding. In cases of organizing pneumonia, reactive type II pneumocyte hyperplasia appears prominently as cuboidal cells lining alveoli while the tissue attempts repair after damage. This pattern can follow infections, drug reactions, or connective tissue diseases. Reactive changes in bronchial epithelium often accompany chronic bronchitis or smoking-related injury, with goblet cell hyperplasia and mild squamous metaplasia as the lining adapts to ongoing irritation.
In interstitial lung disease biopsies, reactive pneumocyte atypia can be prominent near areas of fibrosis or inflammation, sometimes raising concern for malignancy until special stains or clinical correlation confirm its benign nature.
Post-radiation or chemotherapy lung samples classically show reactive atypia with enlarged, bizarre nuclei that mimic cancer but represent healing. Hypersensitivity pneumonitis or resolving infections may display reactive bronchiolar and alveolar changes alongside granulomas or chronic inflammation. Patients searching for “reactive changes lung biopsy” frequently ask if this indicates permanent scarring or progressive disease.
Many reactive patterns are fully reversible if the trigger is eliminated, such as stopping an offending medication, treating infection, or avoiding allergens. In fibrotic conditions, reactive changes highlight ongoing repair attempts that may eventually lead to scarring if unchecked. Specialized pathology consultation integrates these microscopic reactive features with the patient’s exposure history and imaging to differentiate simple repair from more concerning processes, guiding appropriate therapy such as corticosteroids, antifibrotics, or supportive care.
Answering the Most Common Questions About Reactive Changes on Biopsies
Patients across GI, breast, and lung sites share similar concerns when they see “reactive changes” in their report. Does this mean cancer or precancer? Almost never, reactive changes reflect the body’s attempt to heal rather than malignant transformation, though pathologists remain vigilant to exclude dysplasia or carcinoma. What causes reactive changes?
Common triggers include acid reflux or NSAIDs in the GI tract, trauma or prior biopsies in the breast, and smoking, infections, drugs, or radiation in the lungs. Will it go away? Most reactive changes resolve once the underlying irritation or injury is addressed, though persistent triggers may require ongoing management. Do I need treatment or follow-up? This depends on the organ and severity, acid blockers for esophageal reactive changes, medication review for gastric gastropathy, observation or imaging for breast findings, and trigger avoidance or anti-inflammatory therapy for lung patterns. How does this affect my long-term health? Isolated reactive changes carry excellent prognosis with minimal impact, while those associated with chronic conditions may need monitoring to prevent complications.
Lifestyle modifications such as smoking cessation, weight management, or avoiding NSAIDs often accelerate resolution. Honest Pathology’s consultations directly answer these questions by reviewing the report in detail, explaining why reactive features appear, and outlining clear implications for each biopsy site.
How Pathology Consultations Empower Patients with Reactive Changes Findings
Seeing “reactive changes” on a biopsy report can still cause uncertainty when the language feels vague or technical. Honest Pathology offers dedicated pathology consultations that demystify these findings for GI, breast, and lung biopsies alike. Patients receive plain-language explanations of the reactive patterns, their likely causes, and how they fit into the broader clinical picture.
This clarity helps individuals engage more effectively with their gastroenterologist, breast specialist, or pulmonologist, ask targeted questions about management, and understand whether reassurance, treatment, or surveillance is most appropriate. In cases where reactive changes overlap with inflammation or other subtle features, expert review ensures nothing is overlooked while preventing over-treatment of benign repair processes.
Reactive changes on biopsies from the gastrointestinal tract, breast, or lungs are overwhelmingly a sign of the body’s natural healing response rather than disease progression. By seeking expert pathology consultation early, patients transform potential worry into informed confidence. Honest Pathology is committed to providing that understanding, ensuring every individual can interpret their biopsy results clearly and navigate their care journey with knowledge, reassurance, and empowerment.