Understanding cancer at its most fundamental level requires looking at chromosomes. Cytogenetic abnormalities, changes in chromosome structure or number, play a critical role in how cancers develop, progress, and respond to therapy. At Honest Pathology, we emphasize the importance of these insights for both clinical decision-making and education in modern pathology.
This article explores cytogenetic abnormalities, answers commonly searched questions, and highlights their relevance in blood cancers and beyond.
Understanding Cytogenetic Abnormalities
Cytogenetic abnormalities are detectable changes in chromosomes, which carry our genetic information. These changes can be numerical, involving gains or losses of chromosomes, or structural, including translocations, deletions, inversions, and duplications.
In cancer, such abnormalities often disrupt the regulation of growth and survival. Genes that normally control cell division can become overactive, while tumor suppressor genes may be lost or silenced. Recognizing these patterns is essential for accurate diagnosis and personalized treatment.
How Cytogenetic Changes Lead to Cancer
Chromosomal changes can directly contribute to cancer by altering key genes. For example, translocations can fuse two genes, creating an abnormal protein that drives proliferation. Deletions can remove tumor suppressors, leaving cells unchecked.
While some abnormalities are triggered by environmental factors or DNA replication errors, most arise spontaneously during a person’s lifetime. Identifying them in patient samples helps pathologists understand disease behavior and tailor clinical strategies.
Why Cytogenetics Matters in Diagnosis
Cytogenetic analysis is vital in modern cancer diagnostics. Many cancers have characteristic chromosomal changes that define the disease and guide treatment decisions.
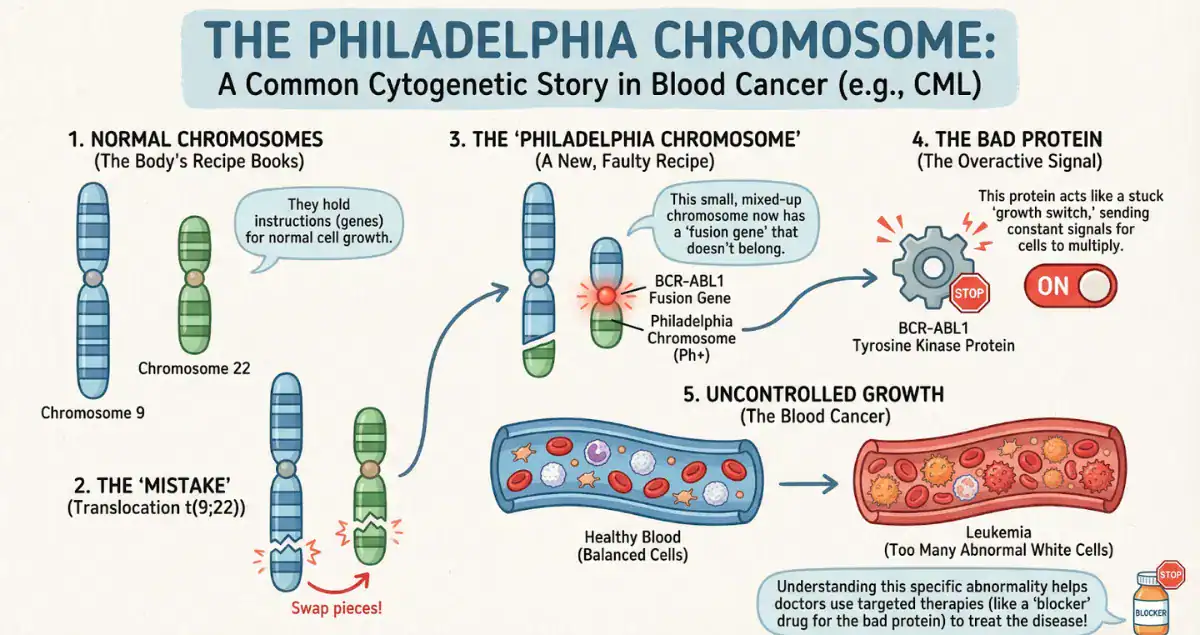
A notable example is the Philadelphia chromosome in chronic myelogenous leukemia, where a translocation between chromosomes 9 and 22 creates a fusion gene driving cancer growth. Detection of this abnormality confirms diagnosis and informs targeted therapy.
Subtle differences in cytogenetic profiles can distinguish between cancers that appear similar under the microscope but behave very differently clinically.
Cytogenetic Abnormalities in Blood Cancers
Blood cancers, such as leukemias and multiple myeloma, provide some of the clearest examples of clinically significant cytogenetic abnormalities.
In acute lymphoblastic leukemia, specific translocations can indicate either favorable or high-risk disease. In acute myeloid leukemia, cytogenetic profiling is central to stratifying patients and guiding therapy. Multiple myeloma also relies on cytogenetic findings, such as deletions or translocations, to determine risk categories and treatment intensity.
These cases illustrate how understanding chromosomal changes is essential for effective patient care.
Landmark Discoveries: The Philadelphia Chromosome
The discovery of the Philadelphia chromosome in chronic myelogenous leukemia revolutionized cancer treatment. This translocation creates a fusion gene that produces a continuously active protein, driving uncontrolled proliferation.
The development of targeted therapies against this abnormal protein exemplifies how cytogenetic insights can translate directly into life-saving treatments. This remains a cornerstone example in the teaching and practice of pathology.
Cytogenetics Beyond Blood Cancers
While blood cancers are most strongly associated with cytogenetic abnormalities, solid tumors also exhibit important chromosomal changes.
In breast cancer, gene amplifications can promote tumor growth and influence therapy selection. In lung cancer, rearrangements can activate oncogenes, providing targets for precision treatments. Advances in testing now allow these abnormalities to be identified with increasing accuracy, expanding the scope of personalized oncology.
Detecting Cytogenetic Abnormalities
Laboratories use multiple techniques to detect chromosomal changes. Traditional karyotyping visualizes entire chromosomes, while fluorescence in situ hybridization targets specific genetic rearrangements.
Next-generation sequencing offers comprehensive genomic profiling, revealing even subtle abnormalities. Mastering these techniques is crucial for pathologists to provide meaningful clinical interpretations.
Prognostic Implications
Cytogenetic findings are among the most powerful predictors of prognosis in cancer. Certain abnormalities indicate favorable outcomes, while others signal aggressive disease or resistance to therapy.
Clinicians use these insights to stratify patients, guiding both treatment decisions and monitoring strategies. Accurate interpretation of cytogenetic data is therefore essential for both planning care and counseling patients.
Cytogenetics and Personalized Medicine
The integration of cytogenetics into clinical practice is a cornerstone of personalized medicine. By identifying the specific chromosomal drivers of a cancer, clinicians can tailor treatment to the individual patient.
Targeted therapies, risk-adapted strategies, and informed monitoring all depend on understanding cytogenetic profiles. This approach improves outcomes while reducing unnecessary treatments.
Looking Forward
The field of cytogenetics continues to evolve rapidly. Emerging technologies allow for faster, more precise detection of abnormalities, and new research is revealing complex interactions between multiple genetic changes in cancer cells.
Artificial intelligence and advanced data analysis promise to further enhance our ability to interpret cytogenetic findings, supporting better patient care and expanding educational opportunities for pathology professionals.
Final Thoughts
Cytogenetic abnormalities provide a window into the biology of cancer, influencing diagnosis, prognosis, and treatment. From the Philadelphia chromosome in chronic myelogenous leukemia to risk stratification in acute myeloid leukemia and multiple myeloma, these changes are essential to modern oncology.
Understanding these abnormalities is not just an academic exercise, it is a practical necessity for effective, personalized patient care. Institutions and educational platforms that focus on pathology and laboratory medicine, like Honest Pathology, continue to play a vital role in translating these insights into clinical practice.