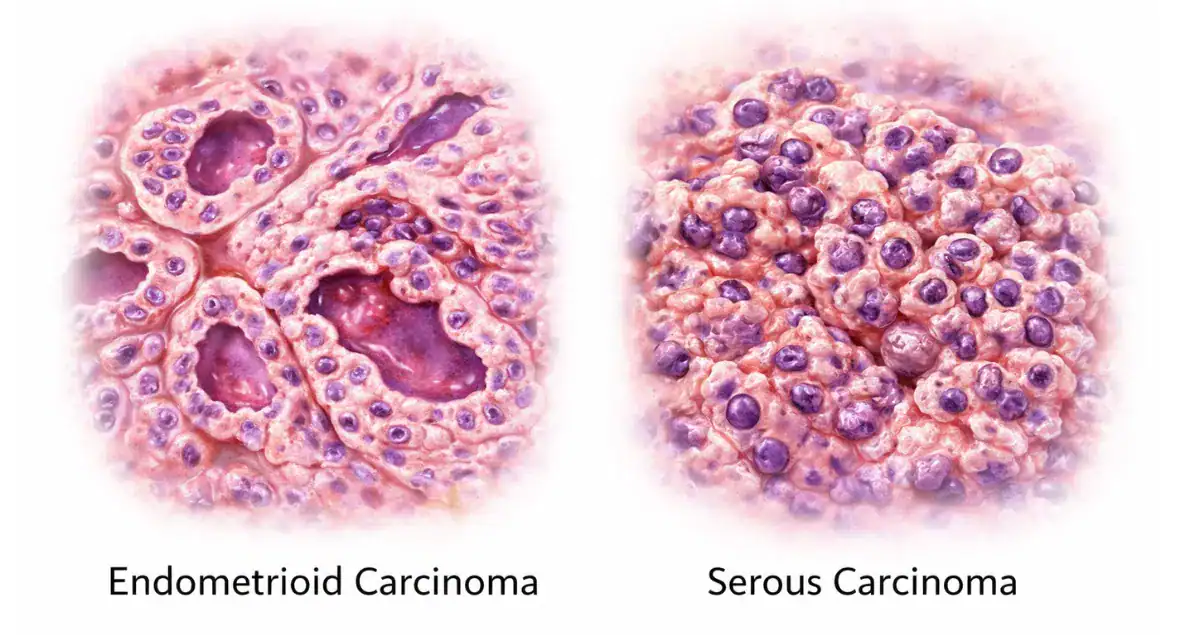
Endometrioid carcinoma and serous carcinoma are two major types of endometrial cancer that differ significantly in biology, behavior, and prognosis. Many patients searching for information about uterine cancer want to understand how these tumor types compare because treatment decisions and survival expectations may vary depending on the diagnosis.
At Honest Pathology, we help patients interpret pathology reports related to gynecologic cancers and explain how microscopic tumor classification influences prognosis and clinical management.
What Is Endometrioid Carcinoma?
Endometrioid carcinoma is the most common type of uterine cancer. It usually develops from the glandular lining of the uterus and is often associated with estrogen-related stimulation.
This tumor type is frequently detected at an earlier stage compared with more aggressive uterine cancers. Endometrioid carcinoma often demonstrates glandular structures that resemble normal endometrial tissue, although the cells show varying degrees of abnormality.
Pathologists assign a tumor grade based on how closely the cancer cells resemble normal glands. Low-grade endometrioid carcinoma tends to grow more slowly and is generally associated with better outcomes.
Many endometrioid tumors are linked to hormonal and metabolic risk factors such as obesity, unopposed estrogen exposure, and certain genetic predispositions.
What Is Serous Carcinoma?
Serous carcinoma is a more aggressive form of uterine cancer. Unlike endometrioid carcinoma, serous carcinoma does not depend on estrogen stimulation and is considered biologically high grade regardless of microscopic appearance.
Serous carcinoma tends to grow more rapidly and is more likely to spread beyond the uterus at the time of diagnosis. Even when tumors appear small, they may demonstrate aggressive behavior due to inherent molecular characteristics.
Microscopically, serous carcinoma shows marked cellular atypia, abnormal nuclear features, and complex growth patterns. These tumors are often treated more aggressively because of their higher metastatic potential.
Differences in Tumor Biology and Behavior
The fundamental difference between endometrioid and serous carcinoma lies in tumor biology.
Endometrioid carcinoma generally develops through a pathway associated with hormonal stimulation and gradual genetic changes. This pathway often allows for detection at earlier stages.
Serous carcinoma arises through different molecular mechanisms and is not typically linked to estrogen exposure. Instead, it is associated with mutations in tumor suppressor genes and high-grade cellular transformation.
Because of these differences, serous carcinoma is usually considered more clinically aggressive even when the tumor is relatively small.
Prognosis: Endometrioid Versus Serous Carcinoma
Prognosis depends on tumor stage, grade, and molecular features, but general patterns are observed across patient populations.
Low-grade endometrioid carcinoma usually carries an excellent prognosis when diagnosed early. Five-year survival rates are high when tumors are confined to the uterus and treated appropriately.
High-grade endometrioid carcinoma behaves more aggressively than low-grade disease but still tends to have a better prognosis than serous carcinoma in many cases.
Serous carcinoma is associated with lower overall survival rates because it has a higher likelihood of spreading beyond the uterus early in the disease process.
However, prognosis is not determined solely by tumor type. Stage at diagnosis remains one of the most important prognostic indicators.
Why Serous Carcinoma Is Considered More Aggressive
Serous carcinoma is characterized by rapid cellular proliferation and early dissemination potential.
Even small serous tumors may show extrauterine spread because of their biological behavior. This is why comprehensive staging is often recommended when serous carcinoma is diagnosed.
Treatment plans may include surgery combined with chemotherapy or radiation therapy depending on stage and clinical risk assessment.
Molecular and Genetic Features
Modern pathology increasingly incorporates molecular classification to refine prognosis.
Endometrioid carcinoma is often associated with mutations affecting pathways related to estrogen signaling and metabolic regulation.
Serous carcinoma frequently demonstrates abnormalities in tumor suppressor genes that regulate DNA repair and cell cycle control.
These molecular differences help explain why serous carcinoma tends to behave more aggressively even when tumor size appears limited.
How Pathology Reports Differentiate These Tumors
Pathologists examine tissue architecture, cellular morphology, and immunohistochemical markers to distinguish tumor types.
Endometrioid carcinoma typically shows gland formation resembling normal endometrial glands.
Serous carcinoma demonstrates more disorganized growth patterns and pronounced nuclear abnormalities.
Accurate classification is critical because treatment strategies depend heavily on tumor subtype.
At Honest Pathology, patient understanding of pathology terminology is emphasized because microscopic classification directly influences management decisions.
Treatment Differences
Treatment approaches vary depending on tumor type and stage.
Endometrioid carcinoma may be managed with surgery alone in early stages, especially when the tumor is low grade and confined to the uterus.
Serous carcinoma is often treated more aggressively because of its higher recurrence risk. Treatment may include surgery followed by systemic therapy or radiation depending on staging results.
The goal of treatment is complete removal of detectable disease and reduction of recurrence risk.
Recurrence Risk
Endometrioid carcinoma has a lower recurrence rate when diagnosed early and treated appropriately.
Serous carcinoma carries a higher risk of recurrence, even after apparently successful treatment, due to its aggressive biological behavior.
Regular follow-up examinations are important for both tumor types because recurrence can sometimes occur years after treatment.
Early detection of recurrence improves the likelihood of effective intervention.
Common Questions About Prognosis
Many patients ask which tumor type is more dangerous. In general, serous carcinoma is associated with a worse prognosis compared with low-grade endometrioid carcinoma.
However, prognosis is highly individualized. Some patients with serous carcinoma do very well with early detection and appropriate treatment.
Another frequent question involves survival expectations. Survival depends on stage, tumor biology, treatment response, and overall health rather than tumor type alone.
Patients also frequently ask whether endometrioid carcinoma can become serous carcinoma. These tumor types arise through different biological pathways, and transformation from one type to another is not considered typical.
Importance of Early Detection
Early detection remains the most important factor in improving outcomes for uterine cancer.
Symptoms such as abnormal uterine bleeding should always be evaluated promptly, particularly in postmenopausal individuals.
Routine gynecologic care and timely diagnostic testing help identify cancer at earlier and more treatable stages.
At Honest Pathology, patient education is considered a critical component of pathology reporting because understanding diagnosis supports better healthcare decisions.
The Bottom Line
Endometrioid carcinoma and serous carcinoma represent two distinct types of uterine cancer with different biological behavior and prognostic implications.
Endometrioid carcinoma is more common and often associated with better outcomes, particularly when detected at low grade and early stage.
Serous carcinoma is less common but generally more aggressive, requiring careful staging and often more intensive treatment.
Accurate pathological classification is essential for prognosis estimation and treatment planning. While tumor type is important, overall prognosis depends on a combination of stage, molecular characteristics, and treatment response.
Understanding the differences between these cancers helps patients interpret pathology reports and communicate effectively with their healthcare providers.