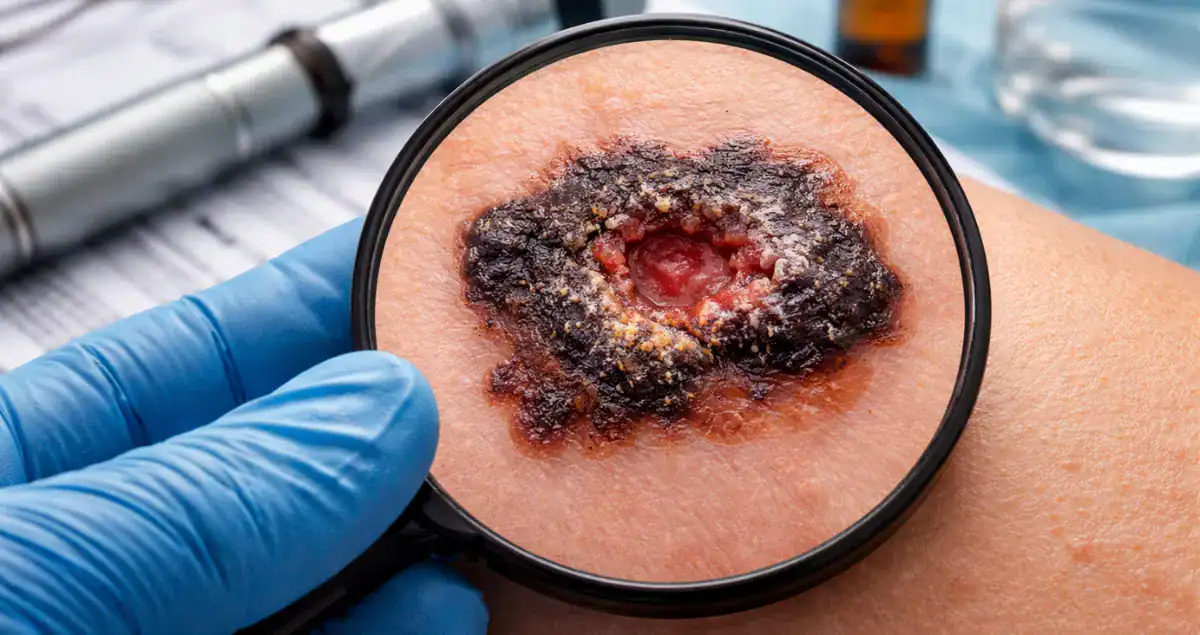
When a pathology report confirms melanoma, one of the most critical terms patients often encounter is ulceration. Ulceration refers to the loss or breakdown of the epidermal layer of the skin overlying the melanoma. While it might appear as a minor microscopic detail, ulceration carries significant implications for staging, prognosis, and clinical management.
At Honest Pathology, we help patients interpret these findings and understand how ulceration fits into the broader context of melanoma care, including why it affects follow-up strategies and, in some cases, the decision to perform sentinel lymph node biopsy.
What Is Ulceration in Melanoma?
Ulceration occurs when the topmost layer of skin over the melanoma is missing. Pathologists distinguish true ulceration from superficial trauma, inflammation, or biopsy-related changes. Only when the epidermis is absent and there is evidence of tumor exposure and associated tissue reaction is ulceration reported.
This finding is significant because it indicates that the tumor has disrupted normal skin barriers. Ulceration is considered a high-risk feature, associated with higher chances of lymph node involvement and potential metastasis compared with non-ulcerated lesions.
How Ulceration Impacts Melanoma Staging
Ulceration is incorporated into the AJCC (American Joint Committee on Cancer) staging system and directly affects the T category, which describes the primary tumor. For example, two melanomas with the same Breslow depth but different ulceration statuses will have different T stages.
A 1.2-millimeter melanoma without ulceration may be staged as T2a, whereas the same thickness with ulceration could be T2b. This higher stage reflects an increased risk of spread and informs follow-up and treatment recommendations.
Ulceration can also influence overall stage grouping. A thin melanoma that would otherwise be considered low-risk may warrant closer monitoring if ulceration is present, highlighting the importance of this feature in clinical decision-making.
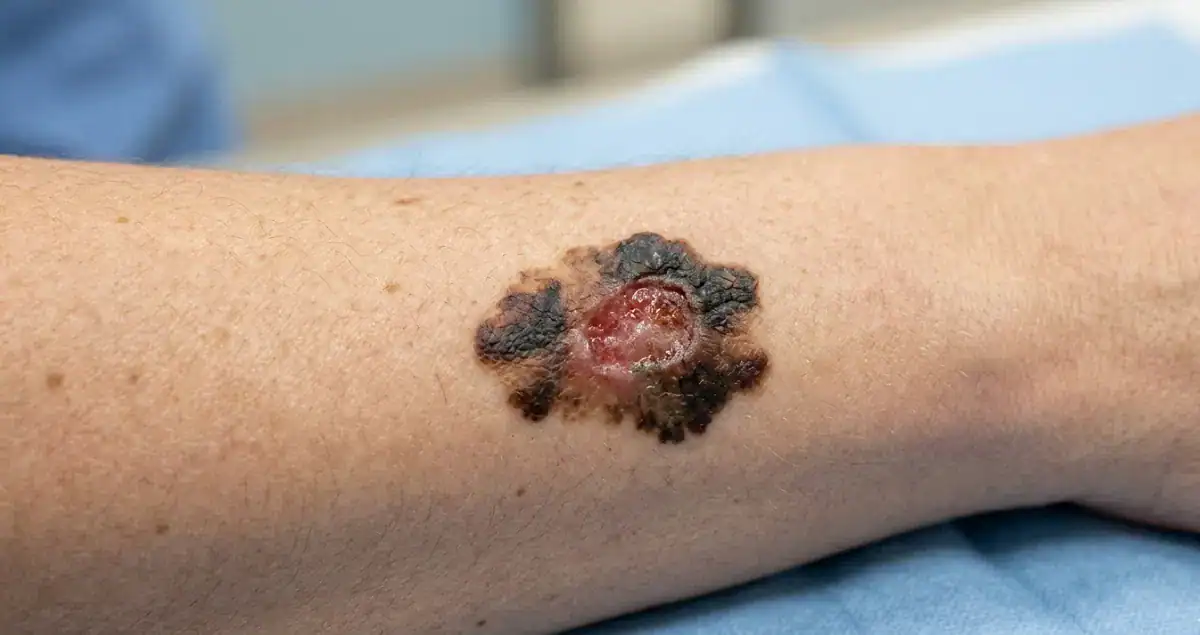 Ulceration and Prognosis
Ulceration and Prognosis
The presence of ulceration is associated with a worse prognosis than a non-ulcerated melanoma of the same thickness. Studies have shown that ulcerated melanomas have higher rates of local recurrence, lymph node metastasis, and distant spread.
However, ulceration does not automatically indicate a poor outcome. Many ulcerated melanomas are detected early, fully excised, and successfully monitored. Early detection, surgical removal, and careful follow-up often lead to excellent long-term outcomes.
For thinner melanomas, ulceration plays a particularly important role in determining whether sentinel lymph node biopsy should be considered. A melanoma under 0.8 millimeters in thickness without ulceration is typically low risk, while the same thickness with ulceration may prompt discussion of nodal evaluation to rule out microscopic spread.
How Ulceration Is Identified
After excision, the melanoma specimen is processed in the pathology laboratory. Tissue is embedded in paraffin, sliced into thin sections, and stained for microscopic evaluation. Pathologists confirm ulceration by observing:
- Absence of the epidermis over the tumor.
- Reactive changes in the surrounding dermis.
- Inflammatory response beneath the missing epidermis.
Differentiating true ulceration from damage caused by biopsy or friction is essential to ensure accurate staging and prognosis.
Ulceration and Surgical Management
While ulceration does not typically change the technique for excising the primary melanoma, it can influence the recommended surgical margins and follow-up strategy. Margins are guided primarily by Breslow depth, but ulceration provides additional context for risk assessment.
For instance, a thin ulcerated melanoma may require more careful attention to achieving clear margins. Deeper or thicker ulcerated melanomas may also prompt closer monitoring for regional lymph node involvement.
Sentinel Lymph Node Biopsy and Ulceration
One of the most common clinical decisions influenced by ulceration is whether to perform a sentinel lymph node biopsy. Sentinel lymph node biopsy is used to determine whether melanoma cells have spread beyond the primary site.
For thin melanomas without ulceration, sentinel node biopsy is often unnecessary due to the very low risk of spread. However, if ulceration is present, even in thin lesions, sentinel lymph node biopsy may be recommended to identify microscopic metastases. This provides valuable staging information and helps guide follow-up care.
Interaction With Breslow Depth and Clark Level
Ulceration is most meaningful when considered alongside Breslow depth, which measures vertical thickness in millimeters, and Clark level, which describes anatomical depth of invasion into the skin layers.
For thin melanomas, combining ulceration with Clark level can help stratify risk. For example, a 0.6-millimeter melanoma confined to the papillary dermis (Clark II) without ulceration carries minimal risk, while the same thickness invading the reticular dermis (Clark IV) with ulceration carries a higher risk and may prompt more aggressive management.
Breslow depth remains the primary predictor of prognosis, but ulceration provides additional nuance that can influence treatment and follow-up.
Misconceptions About Ulceration
Patients often worry that the presence of ulceration means their melanoma is advanced or aggressive. While ulceration is considered high-risk, it does not automatically indicate a poor outcome. Many ulcerated melanomas are small, detected early, and effectively treated with surgery.
It is also important to understand that not every lesion that appears raw, scabbed, or irritated is ulcerated in pathological terms. Pathologists carefully evaluate tissue sections to distinguish true ulceration from trauma or artifact.
How Ulceration Appears in Pathology Reports
A typical melanoma pathology report might read: “Superficial spreading melanoma, Breslow depth 1.1 mm, ulceration present, mitotic rate 2/mm², Clark level III, negative margins.”
This format provides a comprehensive overview of tumor thickness, ulceration, mitotic activity, anatomical invasion, and surgical margins. At Honest Pathology, we help patients understand these findings and their implications for staging, prognosis, and follow-up.
Ulceration and Follow-Up
Patients with ulcerated melanomas generally undergo closer follow-up than those with non-ulcerated lesions of similar thickness. This can include:
- Periodic skin exams to monitor for recurrence or new lesions.
- Sentinel lymph node evaluation when indicated.
- Imaging studies for higher-risk or thicker tumors.
Close follow-up ensures that any recurrence or regional spread is detected early, improving outcomes.
Key Takeaways About Ulceration
- Ulceration refers to the loss of the epidermis overlying a melanoma.
- It is considered a high-risk feature and is incorporated into the AJCC staging system.
- Ulceration increases the likelihood of lymph node involvement and local recurrence but does not automatically indicate a poor outcome.
- Its presence can influence decisions about sentinel lymph node biopsy, surgical margins, and follow-up care.
- Ulceration should always be interpreted in the context of Breslow depth, Clark level, mitotic rate, and other pathological features.
At Honest Pathology, we focus on explaining ulceration in a way that makes sense to patients, showing how it fits into the overall assessment and what it means for treatment planning and prognosis. Understanding ulceration can help patients feel informed and empowered as they work with their healthcare team.