If you’ve ever had a colon polyp removed, it’s natural to wonder whether it can come back, or if new polyps might form elsewhere in your colon. Understanding colon polyp recurrence is important for maintaining long-term colon health and reducing the risk of colorectal cancer. Different types of polyps carry different levels of risk, and knowing what these findings mean helps you and your healthcare team plan follow-up care.
At Honest Pathology, we guide patients in interpreting their pathology reports, explaining the likelihood of recurrence and the steps that can help prevent future problems.
What Colon Polyps Are and Why They Matter
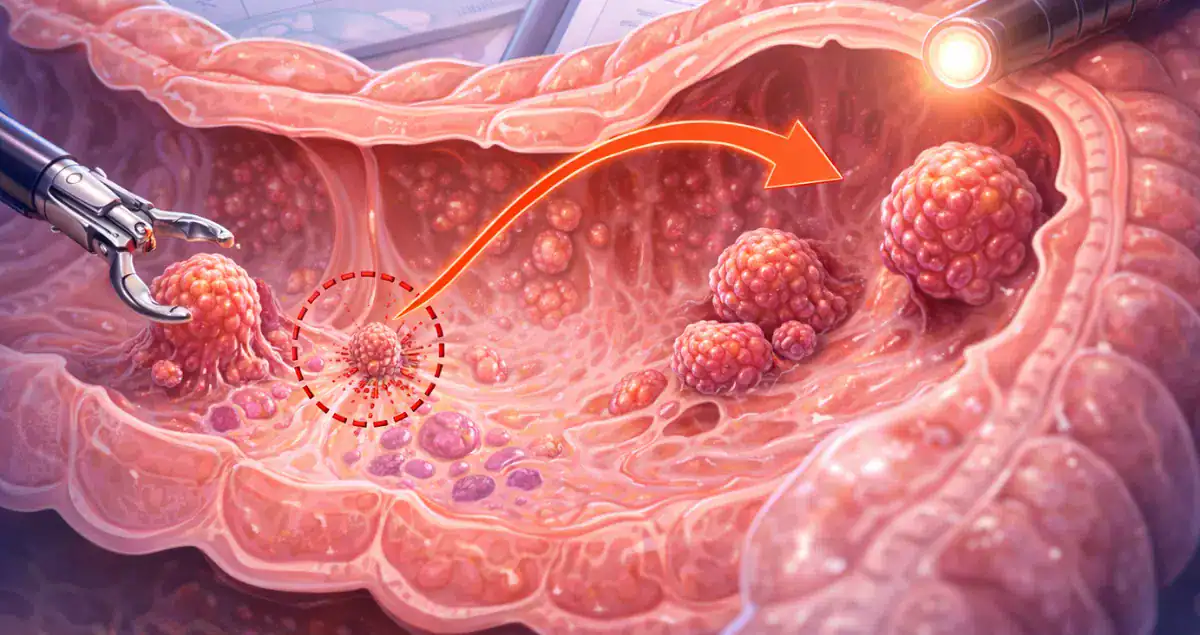
Colon polyps are growths on the inner lining of the colon or rectum. They are quite common and can vary in size, shape, and potential to develop into cancer. Tubular adenomas are one of the most common types. These polyps are considered precancerous, meaning that while they are not cancer, some may develop into cancer over time if left untreated. Hyperplastic polyps are generally benign and rarely become cancerous, particularly when they are small and located in the distal colon. Another important type that may appear in reports is high-grade dysplasia. High-grade dysplasia is a more advanced precancerous change, meaning the cells are more abnormal and have a higher chance of turning into cancer if they are not removed or monitored.
Even when polyps are removed, their presence indicates that the colon is capable of forming new growths, which is why regular follow-up is essential.
 Recurrence of Tubular Adenomas
Recurrence of Tubular Adenomas
For tubular adenomas, studies show that after removal, between 10 and 30 percent of patients may develop a new adenoma within three to five years. The risk is influenced by factors such as the size and number of polyps removed. Larger adenomas or multiple polyps carry a higher chance of new growths forming. Recurrence generally refers to new polyps developing in other areas of the colon rather than the original polyp growing back. This is why follow-up colonoscopy is so important—it allows doctors to detect and remove new polyps before they can develop further.
Recurrence of Hyperplastic Polyps
Hyperplastic polyps are usually low-risk, especially when they are small and located in the lower part of the colon. The recurrence rate for individual hyperplastic polyps is low, and these polyps rarely progress to cancer. However, patients with multiple or larger hyperplastic polyps may need closer monitoring, as these can sometimes indicate a tendency for polyps to form more easily in the colon. Overall, hyperplastic polyps are considered less concerning than adenomas, but keeping up with regular colonoscopy ensures that any new growths are identified promptly.
High-Grade Dysplasia: Recurrence and Risk
High-grade dysplasia carries a higher level of cellular abnormality compared to typical adenomas. It is considered more advanced precancerous tissue. The risk of a polyp with high-grade dysplasia recurring after removal is similar to other adenomas, though slightly higher if multiple polyps were present or if the polyp was large. Importantly, high-grade dysplasia has a greater chance of progressing to invasive cancer if left untreated, which is why careful removal and ongoing surveillance are critical. Even after removal, patients are advised to follow a regular colonoscopy schedule, as new polyps may still form elsewhere in the colon.
Recurrence of Polyps in General
Regardless of type, having had a colon polyp removed increases the chance that new polyps may develop over time. Research indicates that between 20 and 40 percent of patients may develop another polyp within three to five years. Age, family history of colorectal cancer, lifestyle factors like smoking or low-fiber diets, and the presence of multiple polyps at the initial colonoscopy all influence recurrence. Most new polyps are detected early through routine surveillance colonoscopy, and timely removal is highly effective at preventing progression to cancer.
Why Follow-Up Matters
Follow-up colonoscopy is the most effective way to prevent colorectal cancer after a polyp has been removed. The timing of repeat colonoscopy depends on factors such as the size, number, and type of polyps removed, as well as whether high-grade dysplasia was present. Small, single tubular adenomas may be rechecked after five to ten years, while larger or multiple adenomas, or polyps with high-grade dysplasia, may require re-examination in three years. Hyperplastic polyps generally do not require shortened intervals unless multiple or large lesions are found. Following these recommendations ensures that any new polyps are detected and removed before they pose a significant risk.
Addressing Patient Concerns About Recurrence
Many patients worry that a polyp might grow back in the same spot. In most cases, recurrence refers to new polyps forming in other parts of the colon, rather than regrowth of the removed polyp. Another common concern is whether recurrence means cancer is inevitable. The answer is no. With proper polyp removal and adherence to surveillance schedules, the majority of patients maintain long-term colon health. Regular monitoring allows doctors to remove polyps early, preventing progression to cancer.
Moving Forward After Polyp Removal
Having a colon polyp removed is a proactive step in preventing colorectal cancer. Patients with tubular adenomas, high-grade dysplasia, or multiple polyps should adhere to recommended follow-up colonoscopies, maintain healthy lifestyle habits, and communicate any new symptoms to their healthcare team. At Honest Pathology, we help patients interpret their pathology reports, understand the implications of recurrence, and take an active role in their colon health. Understanding these risks empowers patients to stay informed and proactive in preventing future complications.