A prostate core biopsy can feel intimidating when it is recommended or appears in your pathology report. Many men have questions about the procedure itself, the possible findings, and how it affects future care. A prostate core biopsy involves removing small samples of prostate tissue so a pathologist can examine them for abnormal cells, including cancer. Understanding the procedure, what to expect during recovery, and how the results inform patient care can reduce anxiety and help men feel more confident navigating their health.
At Honest Pathology, we guide patients through understanding their biopsy results, whether the report shows high-grade prostatic intraepithelial neoplasm, prostate cancer, or other benign changes.
What a Prostate Core Biopsy Is and Why It Matters
A prostate core biopsy is a procedure in which a doctor removes small cylinders of tissue from the prostate to examine them under a microscope. The biopsy allows pathologists to determine if abnormal cells are present, whether these are cancerous, precancerous, or benign.
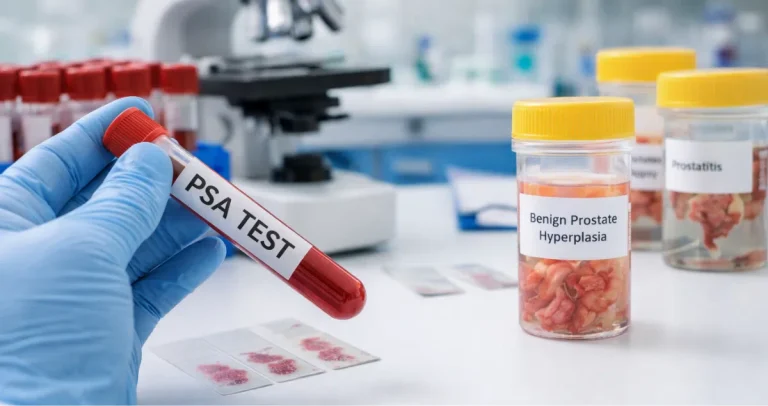
Biopsies are usually recommended when there is elevated PSA, abnormalities on a digital rectal exam, or suspicious findings on imaging tests such as multiparametric MRI. Even if imaging shows irregularities, only a biopsy can confirm whether cancer cells are present.
The biopsy results provide crucial information for doctors to assess the patient’s risk and develop a monitoring or treatment plan. For example, the presence of high-grade prostatic intraepithelial neoplasm indicates abnormal cells that are not yet cancer but may signal increased risk over time.
How the Prostate Core Biopsy Procedure Works
The biopsy is usually performed in a clinic or hospital setting with local anesthesia to reduce discomfort, though sedation may sometimes be offered. The most common method is transrectal ultrasound-guided biopsy, in which a small probe is inserted into the rectum to visualize the prostate. A thin needle then removes small tissue cores from different regions of the prostate to ensure representative sampling.
An alternative method is the transperineal approach, where the needle is inserted through the skin between the scrotum and anus. This approach may reduce the risk of infection and is increasingly used in modern practice. The number of cores typically ranges from ten to twelve, but the exact number depends on prostate size, PSA levels, and other clinical considerations.
After the tissue is collected, it is sent to a pathology lab for careful examination. Each core is analyzed for abnormal cells, including high-grade prostatic intraepithelial neoplasm or cancer, and the findings are compiled into a pathology report.
What to Expect During and After the Biopsy
Most men feel mild pressure or cramping during the biopsy, though severe pain is uncommon. The local anesthesia usually makes the procedure tolerable, and the process itself is relatively quick. After the procedure, patients may notice minor bleeding in the urine, rectum, or semen for a few days, as well as slight soreness or swelling at the biopsy site. Temporary difficulty urinating can occur, but it generally resolves on its own.
In rare cases, infection can develop after a biopsy, which is why doctors often prescribe antibiotics as a precaution. Patients are encouraged to report any fever, worsening pain, or persistent bleeding, as these may indicate the need for prompt medical attention. Understanding the expected recovery process helps reduce worry and prepares patients for what is normal after a biopsy.
Interpreting Prostate Biopsy Results
Pathology reports from a prostate biopsy may indicate normal prostate tissue, benign conditions, precancerous lesions, or cancer. For example, high-grade prostatic intraepithelial neoplasm is a precancerous condition in which abnormal cells are confined to the prostate ducts. It signals an increased risk of developing prostate cancer but is not cancer itself.
When prostate cancer is detected, the report includes important information about the grade and extent of involvement. The Gleason score and Grade Group describe how aggressive the cancer cells appear under the microscope, which helps doctors plan monitoring or treatment.
Some men may find cancer in only a small portion of one core, while others may have multiple cores showing cancer. Each detail helps determine whether active surveillance, surgery, radiation, or another therapy is appropriate.
 How a Prostate Biopsy Guides Care Decisions
How a Prostate Biopsy Guides Care Decisions
The biopsy results are one piece of a larger clinical picture. Doctors consider PSA levels, digital rectal exam findings, imaging results, and biopsy pathology to make individualized recommendations.
For patients with high-grade prostatic intraepithelial neoplasm, a biopsy may not require immediate treatment but usually leads to closer monitoring. Repeat biopsies are sometimes performed within a year to ensure that cancer has not developed. When cancer is found, the grade, stage, and extent inform whether active surveillance is sufficient or whether intervention is necessary.
Even benign findings provide important information, giving both patients and doctors a baseline for future monitoring and helping rule out cancer as a cause of elevated PSA.
Addressing Concerns About Pain, Risks, and Complications
Many men worry about pain, infection, or complications during a prostate core biopsy. While mild discomfort and minor bleeding are normal, serious complications are rare. Pathologists and clinicians confirm that the biopsy does not spread cancer, and the procedure itself is considered safe.
Some men ask how long results take. Typically, pathology evaluation requires several days to a week, depending on the complexity of the examination and the number of cores collected. Honest Pathology helps patients understand their results once they are available, explaining the meaning of findings in clear, understandable terms.
Recovery and What to Do After a Biopsy
After a prostate core biopsy, it is normal to experience light bleeding or mild soreness. Doctors recommend avoiding strenuous activity for a few days and staying well hydrated to help flush the urinary tract. Sexual activity may be temporarily restricted until bleeding resolves.
Follow-up monitoring often includes PSA testing at regular intervals. If high-grade prostatic intraepithelial neoplasm or other precancerous changes are identified, repeat biopsies may be scheduled. Patients are encouraged to report any unexpected symptoms, such as persistent bleeding, fever, or urinary difficulties, to ensure safe recovery.
Understanding the Long-Term Implications
Prostate core biopsy results influence long-term care decisions. A finding of high-grade prostatic intraepithelial neoplasm may prompt more frequent monitoring, while benign results provide reassurance and guidance for future screening. When cancer is detected, biopsy results are used to plan the most appropriate course of action based on tumor grade and risk factors.
Knowing what the biopsy reveals empowers patients to participate actively in their care. It also provides a baseline for comparing future biopsies or PSA trends, allowing doctors to detect changes early and intervene if necessary.
Moving Forward With Confidence
A prostate core biopsy can feel daunting, but understanding the procedure and its purpose helps reduce anxiety. Whether the pathology report shows benign tissue, high-grade prostatic intraepithelial neoplasm, or prostate cancer, the information is critical for guiding monitoring and treatment decisions.
At Honest Pathology, we help patients interpret their biopsy results in plain language. By explaining what each finding means for risk and follow-up, we enable patients to take proactive steps in managing their prostate health. Understanding your pathology report is the first step toward peace of mind and informed decision-making.