When a pathology report mentions “perineural invasion,” many patients feel alarmed or confused. The phrase sounds intimidating, and without context, it is easy to assume the worst. Perineural invasion is a term that describes how cancer cells interact with nerves, and understanding what it really means can help you make sense of your diagnosis, your prognosis, and your follow-up care.
This article explains perineural invasion in everyday language, focusing on colon cancer, prostate cancer, and head and neck squamous cell carcinoma, while also addressing other cancers where this feature is relevant. It will cover what perineural invasion indicates, how it may influence treatment decisions, and what patients often want to know when they see it in their pathology report.
At Honest Pathology, we help patients understand their pathology findings so they can make informed decisions and feel confident discussing them with their doctors.
What Is Perineural Invasion?
Perineural invasion occurs when cancer cells are seen traveling along or around nerves near the primary tumor. It is a descriptive term used by pathologists after examining tissue under a microscope. The cancer cells do not form a separate type of disease; rather, this finding indicates a specific pattern of local spread.
Nerves are present throughout many tissues in the body, and cancer cells in certain tumors sometimes follow these pathways. Perineural invasion describes local behavior, not distant metastasis. When noted in a pathology report, it usually appears alongside other features such as tumor grade, tumor stage, and lymphovascular invasion.
Why Does Perineural Invasion Occur?
Cancer cells can take advantage of nerves because the nerve sheath can provide a path of least resistance. The surrounding nerve environment may produce chemical signals that attract cancer cells, and the area around nerves may offer a somewhat protected environment, allowing tumor cells to move locally.
It is important to understand that perineural invasion is not caused by anything a patient has done or failed to do. It is a microscopic observation that describes how the tumor behaves in tissue, rather than a measure of overall severity or distant spread on its own.
Perineural Invasion in Colon Cancer
In colon cancer, perineural invasion is considered a high-risk feature. When pathologists see cancer cells surrounding or tracking along nerves in or near the tumor, it is a sign that the cancer may have a greater likelihood of recurring.
For example, consider a patient with stage II colon cancer, where the tumor has penetrated through the muscular layer of the colon but has not spread to lymph nodes. If the pathology report notes perineural invasion, doctors may recommend additional chemotherapy after surgery, even though the lymph nodes are clear. The presence of perineural invasion suggests a higher probability of cancer returning, and therefore influences follow-up care.
Perineural invasion in colon cancer is often seen alongside other concerning features, such as lymphovascular invasion or poor differentiation of the tumor cells. Together, these findings help oncologists develop a more comprehensive treatment plan.
Perineural Invasion in Prostate Cancer
Prostate cancer commonly shows perineural invasion under the microscope. Nerves are abundant in the prostate, and cancer cells frequently appear to track along these nerve pathways. However, its meaning in prostate cancer is different from colon cancer.
Perineural invasion in prostate cancer is not necessarily a sign of aggressive disease. Many men with early-stage, low-grade prostate cancer have perineural invasion in their biopsy, but their long-term prognosis remains favorable. For example, a man with Gleason score 6 (Grade Group 1) prostate cancer and perineural invasion may still be a candidate for active surveillance, which involves regular PSA testing, clinical exams, and follow-up biopsies rather than immediate surgery or radiation.
In higher-grade prostate cancers, perineural invasion may be one of several factors considered when choosing treatment, along with Gleason score, PSA level, tumor stage, and the extent of cancer involvement in biopsy cores. It rarely determines the treatment plan on its own but contributes to a more complete understanding of the tumor’s behavior.
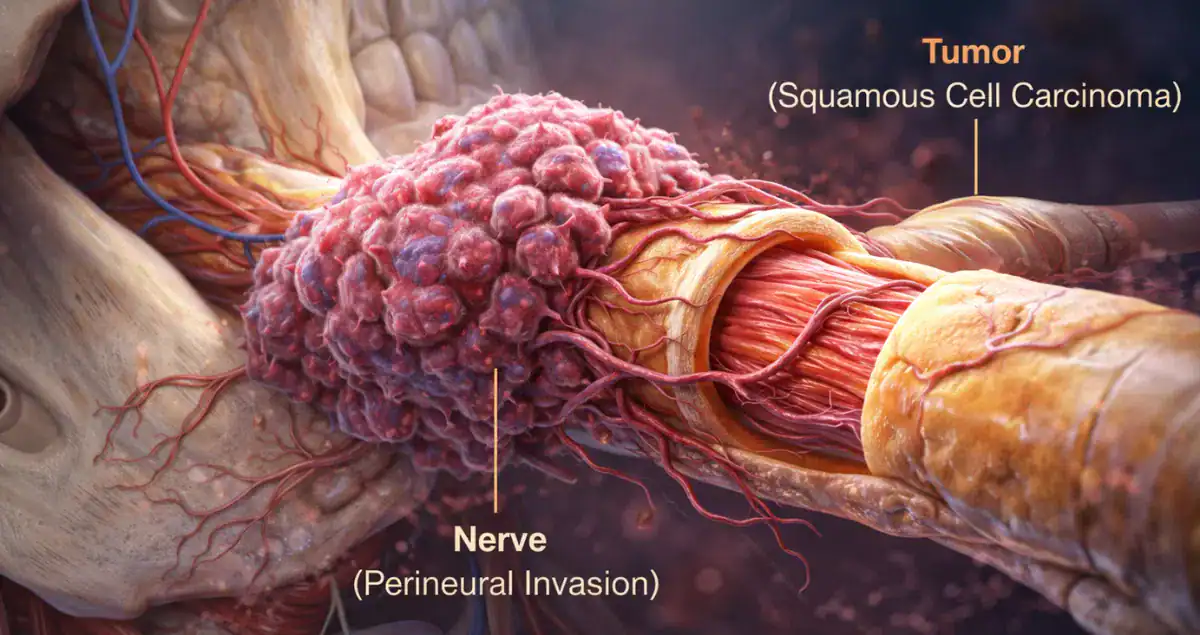 Perineural Invasion in Head and Neck Squamous Cell Carcinoma
Perineural Invasion in Head and Neck Squamous Cell Carcinoma
Head and neck squamous cell carcinoma is a cancer where perineural invasion has particularly important clinical implications. Cancer cells in this region often track along cranial or peripheral nerves, which can lead to local recurrence and, in some cases, involvement of deeper structures such as the skull base or facial nerves.
When perineural invasion is observed in head and neck squamous cell carcinoma, it is generally considered a high-risk feature. It may influence the decision to use adjuvant radiation therapy after surgery, even if the surgical margins are clear, because the presence of tumor cells along nerves increases the chance that microscopic disease remains.
Patients with perineural invasion in this type of cancer may experience symptoms such as numbness, tingling, or weakness in areas supplied by the affected nerve, although small-scale invasion may be asymptomatic. Understanding the presence of perineural invasion helps clinicians tailor treatment, often combining surgery and radiation to reduce recurrence risk.
Perineural Invasion in Other Cancers
Perineural invasion is also observed in pancreatic cancer, melanoma, and some skin cancers such as squamous cell carcinoma. In pancreatic cancer, it is very common and contributes to the characteristic pain associated with the disease. In skin cancers, the presence of perineural invasion can prompt wider surgical margins or additional therapy to reduce the risk of recurrence.
While the clinical significance varies by cancer type, the pattern of tumor cells following nerves provides important information about local tumor behavior and may affect surveillance or treatment planning.
Does Perineural Invasion Mean a Worse Prognosis?
A common question is whether perineural invasion automatically indicates a poor outcome. The answer depends on the type of cancer.
In colon cancer, perineural invasion generally signals a higher risk of recurrence and may prompt consideration of additional treatment, such as chemotherapy, even after a successful surgery. Patients with colon cancer and perineural invasion often require closer follow-up to detect any recurrence early.
In prostate cancer, however, perineural invasion is often present even in low-risk disease. It does not independently predict metastasis or recurrence. Many men with perineural invasion in prostate biopsies do very well over the long term, especially when combined with low Gleason scores and favorable PSA levels.
For head and neck squamous cell carcinoma, the presence of perineural invasion can indicate a need for a more aggressive treatment approach to reduce the risk of local recurrence.
The key point is that perineural invasion should always be interpreted alongside other tumor characteristics. It is one piece of the larger puzzle rather than a definitive predictor of outcome.
How Perineural Invasion Influences Treatment
In colon cancer, perineural invasion may affect decisions about adjuvant chemotherapy. A patient with stage II colon cancer and clear lymph nodes may still be offered chemotherapy if perineural invasion is present, as it suggests a higher risk of recurrence.
In prostate cancer, perineural invasion may influence how closely a patient is monitored, but it is rarely the sole reason to pursue immediate surgery or radiation. Treatment decisions are guided by the combination of tumor grade, PSA levels, and clinical stage.
In head and neck or skin cancers, perineural invasion may prompt wider surgical margins, radiation, or other interventions to reduce the risk of cancer returning along the nerve pathways.
How Is Perineural Invasion Detected?
Perineural invasion is diagnosed when a pathologist examines tissue under a microscope. Cancer cells surrounding or tracking along a nerve are considered perineural invasion. It cannot usually be detected by imaging alone. Sometimes special stains are used to highlight nerve structures, but standard tissue staining often provides sufficient information.
Pathology reports typically describe whether perineural invasion is present within the tumor and whether nerves at the margin of the specimen are involved. For example, a report might read: “Invasive adenocarcinoma with perineural invasion observed. Surgical margins are clear.” This indicates that cancer cells were present along nerves but did not extend to the edges of the removed tissue.
Symptoms Related to Perineural Invasion
In most cancers, including colon and prostate cancer, perineural invasion does not cause specific symptoms. Any symptoms are usually related to the primary tumor itself. In pancreatic cancer, perineural invasion can contribute to pain because of involvement of nerves deep in the abdomen. In head and neck cancers, it may cause numbness, tingling, or discomfort.
Understanding that perineural invasion is often microscopic and symptomless helps reduce unnecessary worry when it is noted in a pathology report.
Does Perineural Invasion Mean Cancer Has Spread?
Perineural invasion does not mean that cancer has spread to distant organs. It describes local tumor behavior along nerve pathways near the tumor. Distant spread, or metastasis, is detected through imaging, blood tests, or findings in lymph nodes or distant tissues.
Patients often mistakenly assume that perineural invasion indicates metastasis, but this is not the case. It is an important feature to guide treatment and predict local recurrence risk, but it is not synonymous with widespread cancer.
Can Perineural Invasion Be Prevented?
There is no way to prevent perineural invasion, as it is a behavior of the cancer itself. Healthy lifestyle choices, cancer screening, and early detection may reduce overall cancer risk, but they do not specifically affect whether a tumor shows perineural invasion under the microscope.
Moving Forward With Confidence
Seeing perineural invasion in a pathology report can feel alarming, but understanding its meaning can reduce unnecessary worry. It is a descriptive finding that reflects how cancer cells behave locally. In colon cancer, it may prompt additional treatment considerations. In prostate cancer, it is common and often does not change the treatment approach. In head and neck squamous cell carcinoma, it may influence surgery or radiation planning to reduce the risk of recurrence.
The most helpful approach is to review the finding with your physician in the context of your overall pathology report, including tumor grade, stage, and other features. Doing so allows you to understand your prognosis and participate confidently in decisions about your care.
At Honest Pathology, we help patients interpret their pathology reports in clear language, explaining what features like perineural invasion mean for treatment planning and long-term outlook. Understanding your report is a crucial step toward peace of mind and proactive management of your health.