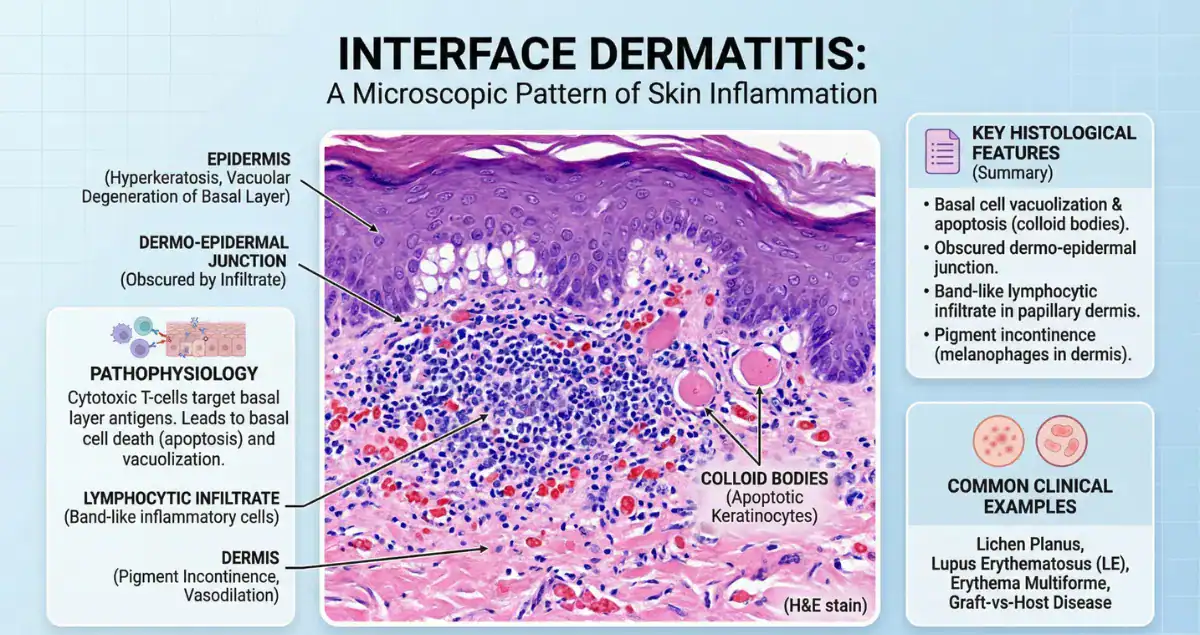
Interface dermatitis is a classic histologic pattern that reflects injury at the junction between the epidermis and dermis, also known as the dermoepidermal junction. This region is critical for skin integrity, and when it becomes a target of immune-mediated damage, a distinctive set of microscopic features emerges. Pathologists recognize interface dermatitis by the presence of lymphocytes along the basal layer of the epidermis, often accompanied by damage to basal keratinocytes.
This damage may appear as vacuolar change, where the basal layer looks disrupted and pale, or as more pronounced cell death, referred to as apoptotic or dyskeratotic keratinocytes. In some cases, the inflammation is dense and obscures the junction entirely. These variations are not just descriptive, they help narrow the diagnostic possibilities.
Importantly, interface dermatitis is not a diagnosis in itself. It is a pattern, and like many patterns in pathology, it must be interpreted in a clinical context. The same basic histologic finding can be seen in autoimmune diseases, drug reactions, infections, and even early neoplastic processes.
The Hallmark Pattern: Why the Dermoepidermal Junction Matters
The dermoepidermal junction is a key site of immune activity in the skin. When lymphocytes target this area, they disrupt the connection between the epidermis and dermis, leading to the characteristic changes seen under the microscope. This process often results in pigment incontinence, where melanin drops into the dermis, and can explain why many of these conditions leave behind areas of hyperpigmentation.
A common question is whether interface dermatitis always indicates an autoimmune disease. While autoimmune conditions are a major cause, the answer is no. The pattern can also be triggered by medications, viral infections, and other inflammatory processes. The challenge for the pathologist is to distinguish among these possibilities using subtle histologic clues.
Lichen Planus: The Prototypical Interface Dermatitis
One of the most well-known conditions associated with interface dermatitis is lichen planus. This disease demonstrates a dense, band-like infiltrate of lymphocytes hugging the dermoepidermal junction. The basal layer shows significant damage, and the overlying epidermis often has a saw-tooth appearance.
Civatte bodies, which are apoptotic keratinocytes, are frequently seen and serve as an important diagnostic clue. The inflammation in lichen planus is typically well-organized and sharply demarcated, making it one of the more recognizable patterns for pathologists.
Clinically, patients present with pruritic, violaceous papules, and the correlation between clinical and histologic findings is often strong. This makes lichen planus a cornerstone example when learning about interface dermatitis.
Lupus Erythematosus: A Subtler but Significant Pattern
Interface dermatitis is also a key feature of cutaneous lupus erythematosus, although the pattern tends to be more subtle than in lichen planus. The lymphocytic infiltrate is often less dense and more patchy, and there is usually accompanying inflammation around blood vessels and adnexal structures.
One distinguishing feature is the presence of increased dermal mucin, which can be highlighted with special stains. The basement membrane may also appear thickened. These additional findings help separate lupus from other interface processes.
Patients and clinicians often wonder whether a biopsy can definitively diagnose lupus. While histology provides strong supportive evidence, it is typically interpreted alongside clinical findings and laboratory tests. This highlights the importance of integrating multiple sources of information in dermatopathology.
Drug Reactions: A Common and Variable Cause
Drug-induced interface dermatitis is another important and frequently encountered category. The histologic pattern can mimic both lichen planus and lupus, sometimes making the distinction challenging. Clues that suggest a drug reaction include the presence of eosinophils, a more mixed inflammatory infiltrate, and less uniform involvement of the dermoepidermal junction.
In some cases, the pattern is referred to as a lichenoid drug eruption because of its resemblance to lichen planus. Identifying this possibility is critical, as discontinuation of the offending medication can lead to resolution of the condition.
A natural question that arises is how pathologists differentiate between idiopathic lichen planus and a drug-induced process. The answer lies in a combination of histologic hints and clinical history, particularly medication exposure.
Viral Exanthems and Other Causes
Certain viral infections can also produce interface dermatitis, typically with a milder and more transient pattern. The infiltrate is often less dense, and the degree of basal cell damage is limited. These cases are usually interpreted in the context of clinical symptoms such as fever or rash.
Other less common causes include graft-versus-host disease, which can show a striking interface pattern with apoptotic keratinocytes, and early erythema multiforme, where scattered necrotic keratinocytes are a key feature.
These variations demonstrate how interface dermatitis serves as a shared pathway for multiple types of skin injury. The underlying cause can differ significantly, but the histologic response converges on the same vulnerable region of the skin.
What Interface Dermatitis Means for Patients
When interface dermatitis is reported on a biopsy, patients often want to know whether it is serious or chronic. The answer depends entirely on the underlying condition. Some causes, such as drug reactions or viral exanthems, may resolve completely. Others, like lichen planus or lupus, may follow a more chronic or relapsing course.
Another common concern is whether the finding is contagious or dangerous. In most cases, interface dermatitis itself is not contagious, though certain underlying causes, like viral infections, may be. The key point is that the histologic pattern does not define the clinical behavior on its own.
Because the terminology can be unfamiliar, many patients seek additional explanation after receiving their pathology report. Understanding what the pattern means, and what it does not mean, is an important step in reducing anxiety and guiding appropriate follow-up.
Why Expert Interpretation Makes a Difference
Interface dermatitis is a classic example of how pattern recognition in pathology must be paired with careful interpretation. Small differences in the distribution of inflammation, the presence of specific cell types, and associated tissue changes can shift the diagnosis from one condition to another.
For patients and clinicians trying to make sense of a pathology report, this level of nuance is not always immediately clear. This is where services like Honest Pathology can provide meaningful support. By translating complex histologic findings into clear, clinically relevant explanations, Honest Pathology helps ensure that important details are understood rather than overlooked.
Whether clarifying the significance of a biopsy result or providing additional context for a diagnosis, having access to expert insight can make the process far less overwhelming.
The Broader Role of Interface Dermatitis in Modern Dermatopathology
As our understanding of immune-mediated skin diseases continues to grow, interface dermatitis remains a central concept in dermatopathology. It represents a shared histologic response to a variety of insults, unified by immune targeting of the dermoepidermal junction.
Advances in immunology and molecular diagnostics are beginning to refine how these conditions are classified and treated. However, the fundamental histologic pattern remains as relevant as ever. Recognizing interface dermatitis and understanding its implications is essential for accurate diagnosis and effective patient care.
Finding Clarity in Your Pathology Report
Encountering a term like interface dermatitis in a pathology report can feel confusing, especially without additional context. While the finding itself is common, its interpretation depends on a range of factors that go beyond the microscope.
Seeking clear, expert explanation is often the best way to gain confidence in what the report means. Honest Pathology offers a resource for patients and clinicians who want straightforward, reliable clarification. By turning complex terminology into understandable insights, it helps bridge the gap between diagnosis and understanding.
In a field where details matter, having that clarity can make all the difference.