Bone marrow is the soft, spongy tissue inside certain bones that acts like a factory for producing blood cells, red cells that carry oxygen, white cells that fight infection, and platelets that help clotting. When something seems wrong with blood counts or when cancer is suspected, doctors turn to a bone marrow biopsy to take a close look inside that factory. This straightforward procedure removes a small sample of marrow so experts can see exactly what is happening at the cellular level. It plays a central role in diagnosing blood cancers, checking whether solid tumors have spread, staging disease, and guiding treatment decisions. The test answers many common questions that arise after abnormal blood work or a cancer diagnosis: why it is needed, what the results actually mean, how uncomfortable it feels, and what comes next. This guide explains everything in everyday language so the process feels less mysterious and more manageable.
If any part of this explanation leaves you wanting more clarity, especially about your own pathology report, services like Honest Pathology offer virtual consultations with board-certified pathologists who review reports line by line, explain terms in plain language, and answer your specific questions directly.
What Is a Bone Marrow Biopsy and Why Is It Performed?
A bone marrow biopsy is a quick medical procedure in which a doctor removes a tiny core of solid marrow tissue, often along with a small amount of liquid marrow through aspiration. Together these samples give a complete picture of how blood cells are being made. The test is ordered when blood tests show unexplained anemia, too many or too few white cells or platelets, or when symptoms point to a problem in blood production. It is especially important for diagnosing or ruling out cancers that start in the bone marrow or spread there. Doctors use the results to confirm a condition, determine how advanced it is, identify the exact type of disease, and decide on the best treatment plan. Many patients wonder whether every cancer requires this test; the answer is no, it is mainly for blood-related cancers and for checking spread in certain solid tumors, but it provides information that blood tests alone cannot.
The Procedure: What Happens During a Bone Marrow Biopsy
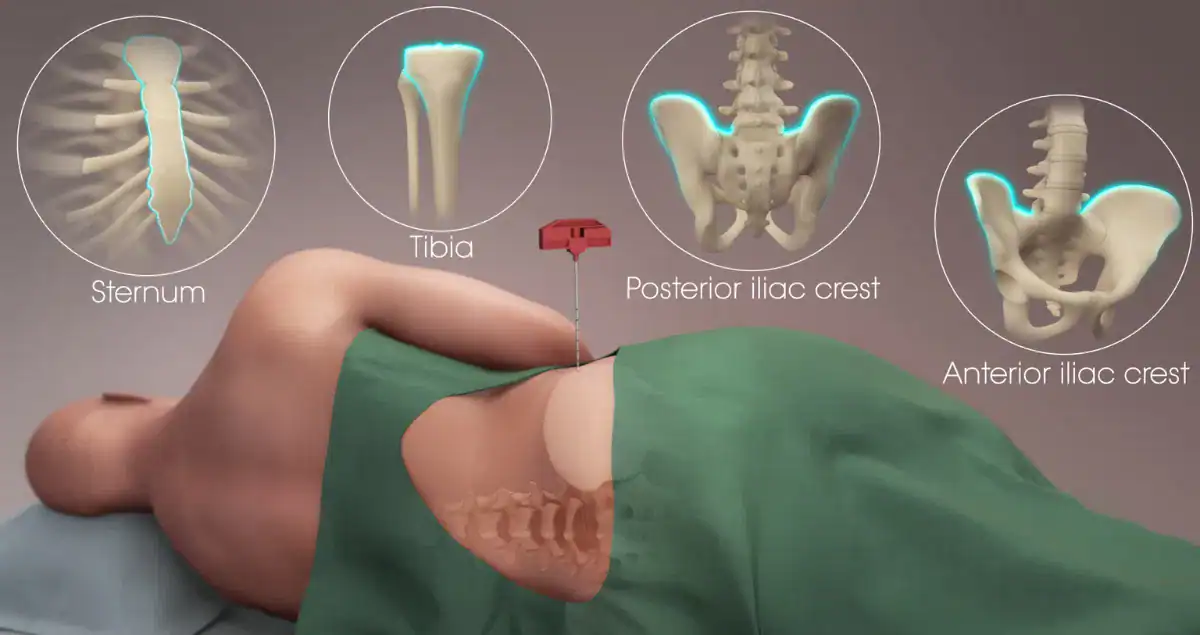
The biopsy usually takes place in a clinic or hospital room and lasts about 10 to 30 minutes. Most people lie on their side while the doctor numbs the skin and the outer layer of bone over the back of the hip with local anesthetic. Once numb, a thin needle draws out the liquid marrow portion first, which can cause a brief sharp pressure or sting lasting just a few seconds. Then a slightly larger needle is used to take the solid core sample, creating a feeling of pressure or a dull ache. Some clinics offer mild sedation or anxiety medication to make the experience calmer. Patients often ask if it hurts badly; most describe it as uncomfortable but tolerable, similar to a deep bruise or a quick toothache, and the numbing medicine keeps pain under control. The site is bandaged afterward, and most people go home the same day.
What Doctors Are Looking for in Bone Marrow Samples
Pathologists examine the samples under a microscope and run additional tests to check several key things. They count the different types of cells and look for any that look abnormal in shape or size. They assess whether the marrow is making the right balance of red cells, white cells, and platelets or if one type is crowding out the others. They search for cancer cells that do not belong there at all, such as immature blast cells or abnormal plasma cells. They also evaluate the overall architecture, how the cells are arranged, because crowding, scarring, or empty spaces can signal serious problems. Genetic tests on the sample can reveal chromosome changes or mutations that help identify the exact disease and predict how it might behave. In short, the biopsy shows whether the marrow factory is healthy, overproducing dangerous cells, or invaded by something it should not contain.
How Bone Marrow Biopsies Help Diagnose and Stage Cancers
The test is a gold-standard tool for blood cancers because it directly samples the place where the disease begins. When blood counts look suspicious, the biopsy confirms whether leukemia, lymphoma, or multiple myeloma is present and provides details that shape treatment. It also stages the cancer by showing how much of the marrow is involved. For people with solid tumors elsewhere in the body, such as breast or prostate cancer, the biopsy checks whether stray cancer cells have traveled to the marrow, which changes the stage and treatment approach. Beyond initial diagnosis, the procedure is repeated during and after therapy to see whether the cancer is responding, whether any hidden disease remains, or whether the marrow has recovered enough to produce healthy blood cells again. This monitoring role is one reason patients often have several biopsies over the course of care.
Bone Marrow Biopsies in Specific Cancers
In leukemia the biopsy reveals whether immature blast cells are taking over the marrow and crowding out normal cells, which explains fatigue, infections, and bleeding. It also identifies the subtype of leukemia and any genetic markers that guide chemotherapy or targeted drugs. For lymphoma the test shows whether the disease has moved from lymph nodes into the marrow, helping doctors decide the stage and whether more aggressive treatment is needed. In multiple myeloma the biopsy measures the percentage of abnormal plasma cells, checks for genetic changes that affect prognosis, and tracks how well treatments are clearing the marrow. In metastatic cancers from other sites the biopsy can be the first clear evidence that the disease has reached the bones, prompting changes in therapy. Across all these cancers the biopsy turns vague blood-test worries into a precise diagnosis and a clear road map forward.
Understanding Bone Marrow Biopsy Results
Results usually come back within a few days for basic findings, though genetic tests can take one to two weeks. A normal report means the marrow looks healthy and is producing the expected mix of cells. An abnormal report might say the marrow contains too many of one cell type, shows scarring, or contains cancer cells. The percentage of abnormal cells, the presence of specific mutations, and the overall cellularity all give doctors the information they need to choose or adjust treatment. Many people worry about what a “positive” result means; it simply means something abnormal was found, which could be cancer, a treatable blood disorder, or even an infection that needs antibiotics. The report also rules things out, which can bring relief even when further steps are required. Pathologists include clear explanations, but the language can still feel technical at first.
Risks, Pain Management, and Recovery
Complications are rare. The most common side effect is soreness at the biopsy site that lasts a few days to a week and feels like a deep bruise. Mild bleeding or bruising can occur, and a pressure bandage helps control it. Infection is possible but uncommon when proper sterile technique is used. Serious problems such as prolonged bleeding or damage to nearby structures are extremely rare. Most patients manage discomfort with over-the-counter pain relievers and by avoiding heavy lifting for a day or two. Recovery is quick, many people return to normal activities the next day, and the small scar fades over time. Patients frequently ask how long they will feel the effects; the answer is usually less than a week, and the information gained from the test far outweighs the temporary discomfort.
The Role of Bone Marrow Biopsy in Ongoing Treatment and Monitoring
After diagnosis the biopsy becomes a tool for tracking progress. Follow-up tests show whether treatment is clearing cancer cells from the marrow, whether normal blood production is returning, or whether minimal residual disease remains that requires more therapy. In some blood cancers doctors repeat the procedure at set intervals to catch any changes early. The results also help decide when it is safe to reduce treatment or move to maintenance therapy. This ongoing use turns the biopsy from a one-time scare into a reliable way to stay ahead of the disease.
In the end, a bone marrow biopsy takes the guesswork out of blood and cancer problems by letting doctors see exactly what is happening inside the body’s blood-cell factory. While the idea of the procedure can feel intimidating, it is short, well-controlled, and provides answers that shape the best possible care. The results often bring clarity and a path forward even when they confirm a serious diagnosis. If you or a loved one has a bone marrow biopsy report in hand and want help understanding every detail, from cell counts to genetic findings to what it means for treatment, consider reaching out to experts at Honest Pathology, who specialize in translating complex pathology reports into clear, actionable information for patients. This knowledge empowers better conversations with the medical team and greater confidence moving ahead.
Image Credit: Scientific Animations
Scientific Animations (CC BY 4.0) Cropped