Atypical cells in urine cytology reports are among the most common and anxiety-provoking findings patients encounter during bladder cancer screening or follow-up. When the pathology description notes “atypical urothelial cells,” many individuals immediately worry that cancer is present or imminent, yet the vast majority of these results do not represent malignancy. Urine cytology examines shed cells from the urinary tract under the microscope to detect abnormal changes, and the term “atypical” describes cells that look neither completely normal nor clearly cancerous. This indeterminate category exists because inflammation, infection, stones, or recent procedures can mimic early neoplastic changes. Honest Pathology provides expert pathology consultations that translate these nuanced reports into straightforward language, empowering patients to understand their specific findings, assess real cancer risk, and make confident decisions about next steps.
What Are Atypical Cells in Urine Cytology?
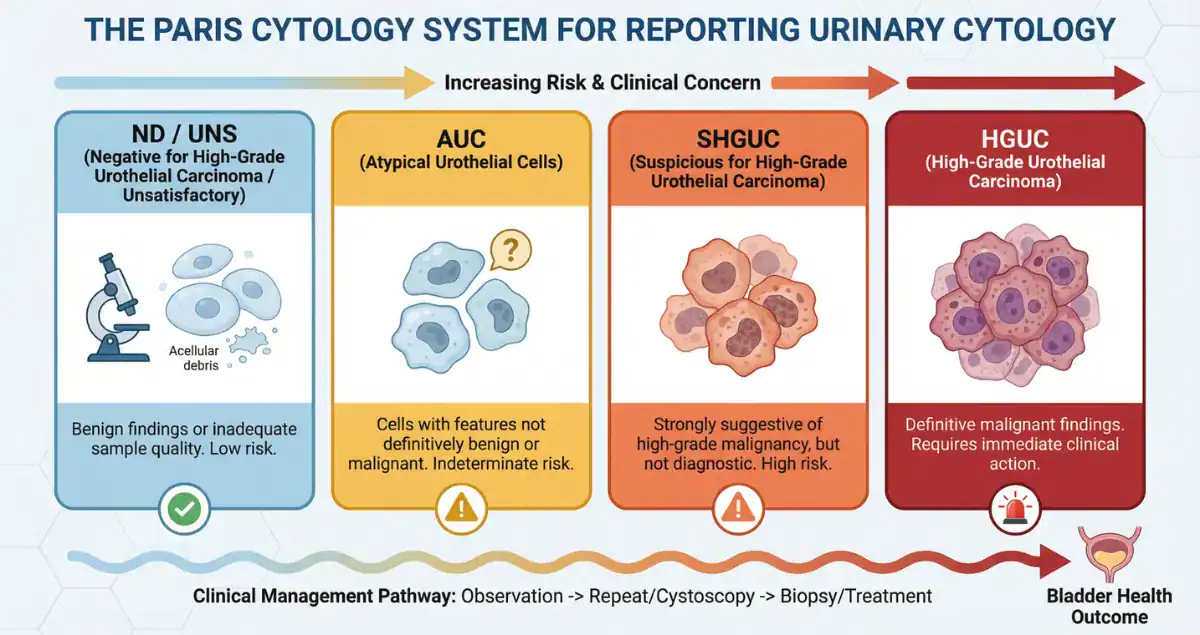
Urine cytology involves collecting a urine sample, concentrating the cells, and staining them for microscopic review. Normal urothelial cells are uniform in size and shape with small, regular nuclei. Atypical cells show mild nuclear enlargement, slight irregularity in nuclear contours, or increased nuclear-to-cytoplasmic ratio that falls short of the criteria for outright malignancy. Pathologists use standardized systems such as the Paris System for Reporting Urinary Cytology to categorize these changes. The “atypical urothelial cells” (AUC) category is deliberately broad to avoid missing early high-grade lesions while preventing over-diagnosis. In practice, most atypical findings are reactive rather than neoplastic. Patients often feel alarmed by the word “atypical,” yet pathology consultation helps clarify that this designation reflects uncertainty rather than confirmed cancer.
Common Causes of Atypical Cells Beyond Cancer
A wide range of non-cancerous conditions can produce atypical cells in cytology. Urinary tract infections, stones, or recent instrumentation such as catheterization frequently cause reactive changes that mimic early neoplasia. Chronic inflammation from conditions like interstitial cystitis or radiation cystitis can also lead to persistent atypia. In smokers or individuals exposed to certain chemicals, mild cellular alterations may appear even without a tumor. Benign prostatic hyperplasia in men and vaginal atrophy in women sometimes shed atypical-appearing cells into the urine. Because these causes are far more common than malignancy, pathologists emphasize clinical correlation. Honest Pathology reviews the full context of the cytology slide and any accompanying biopsy or history, helping patients see whether their atypical cells are more likely explained by a treatable benign process than by cancer.
 How Pathologists Distinguish Atypical from Suspicious or Malignant Cells
How Pathologists Distinguish Atypical from Suspicious or Malignant Cells
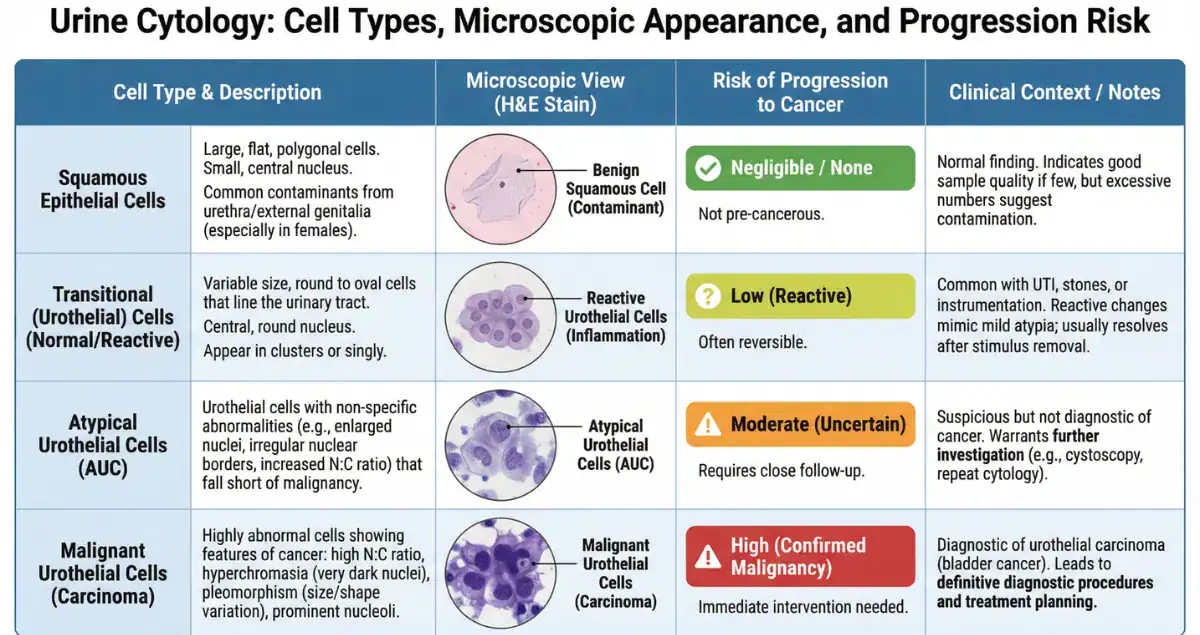
The microscopic spectrum in urine cytology ranges from negative through atypical, suspicious, to high-grade urothelial carcinoma. Atypical cells display only subtle abnormalities and lack the coarse chromatin, irregular nuclear membranes, or high nuclear-to-cytoplasmic ratios required for a suspicious or malignant diagnosis. Suspicious for high-grade urothelial carcinoma (SHGUC) shows more pronounced changes, while definitive malignant cells exhibit marked pleomorphism and mitotic activity. The distinction matters because management escalates with each category. Most atypical results do not progress, but the finding prompts further evaluation to rule out hidden lesions that cytology might have missed. Honest Pathology consultations highlight the precise features that place a case in the atypical category versus higher-risk groups, giving patients a clear understanding of why their report reads as it does and what that implies for immediate risk.
The Actual Risk of Progression to Bladder Cancer
The cancer risk associated with atypical cells in urine cytology is low but not zero, and it varies with patient history. In individuals with no prior bladder cancer, the risk of detecting high-grade urothelial carcinoma on subsequent cystoscopy or biopsy is approximately 8 to 15 percent. When atypical cells are found during routine surveillance in patients with a previous history of bladder cancer, the risk rises to roughly 20 to 30 percent for high-grade disease on follow-up. Over a 10-year period, the cumulative risk of developing bladder cancer after an isolated atypical result without other risk factors remains under 5 percent in most low-risk patients, but it can reach 15 to 25 percent in those with heavy smoking history, occupational exposures, or persistent atypia on repeat cytology. Importantly, the large majority of atypical findings never progress to cancer; many resolve spontaneously or after treatment of underlying inflammation. Factors that increase risk include older age, male sex, smoking, and repeated atypical results. Honest Pathology helps patients interpret their personal risk by reviewing the cytology in light of clinical history, explaining why one atypical report may warrant simple repeat testing while another prompts earlier cystoscopy.
Recommended Follow-Up After an Atypical Cytology Result
An atypical cytology report almost always leads to additional evaluation rather than immediate alarm. Guidelines typically recommend repeat cytology in three to six months combined with cystoscopy to visualize the bladder lining directly. If cystoscopy is normal and atypia persists, further tests such as enhanced imaging or molecular urine markers may be considered. In low-risk patients with a single atypical result and normal cystoscopy, surveillance can often return to routine intervals. Patients frequently wonder how often they will need testing and whether an atypical result means lifelong intensive monitoring. The answer depends on the overall clinical picture and whether high-grade features are ever identified. Honest Pathology consultations provide a clear roadmap by explaining the cytology findings alongside any available biopsy results, helping patients understand the rationale for each recommended test and when the risk profile may allow de-escalation of surveillance.
Why Atypical Cells Do Not Always Mean Cancer Is Present or Imminent
Many patients search for reassurance that atypical cells equate to cancer, and the evidence is reassuring. The majority of atypical cytology cases represent reactive or inflammatory changes rather than neoplasia. Even when early dysplasia or carcinoma in situ is present, cytology often detects it before invasive cancer develops, allowing intervention at a highly curable stage. The 10-year outlook for patients whose atypical cells are thoroughly evaluated and found to be benign remains excellent, with cancer risk comparable to the general population once inflammation is controlled. Honest Pathology emphasizes these distinctions during consultations, showing patients the specific cellular features that separate reactive atypia from true precancerous changes and outlining why most people with this finding never develop bladder cancer.
How Honest Pathology Empowers Patients Facing Atypical Urine Cytology Results
Receiving a cytology report that mentions atypical cells can feel vague and frightening when the language is technical and the next steps unclear. Honest Pathology offers focused pathology consultations that demystify every aspect of the report: the degree of atypia, the presence or absence of worrisome nuclear features, and how these findings translate into real-world cancer risk. Patients gain a personalized explanation of whether their atypia is likely reactive or merits closer attention, along with practical guidance on questions to ask their urologist about cystoscopy timing, repeat testing, and lifestyle modifications such as smoking cessation. This clarity transforms uncertainty into informed confidence, enabling patients to advocate effectively for appropriate care while avoiding unnecessary procedures or prolonged worry. In a test used both for screening and lifelong surveillance, expert pathology insight is the key to understanding results in context rather than in isolation.
Atypical cells in urine cytology represent an indeterminate but common finding that prompts careful evaluation rather than panic. While a small percentage of cases will ultimately reveal high-grade urothelial carcinoma, the large majority reflect benign reactive changes or low-risk conditions that resolve or remain stable with proper follow-up. By providing clear, individualized interpretations of cytology reports and realistic risk assessments, Honest Pathology equips patients with the knowledge needed to navigate the next steps confidently. Whether the atypia is an isolated finding or part of ongoing surveillance, accurate pathology insight helps individuals focus on controllable factors and move forward with peace of mind about their urinary tract health.