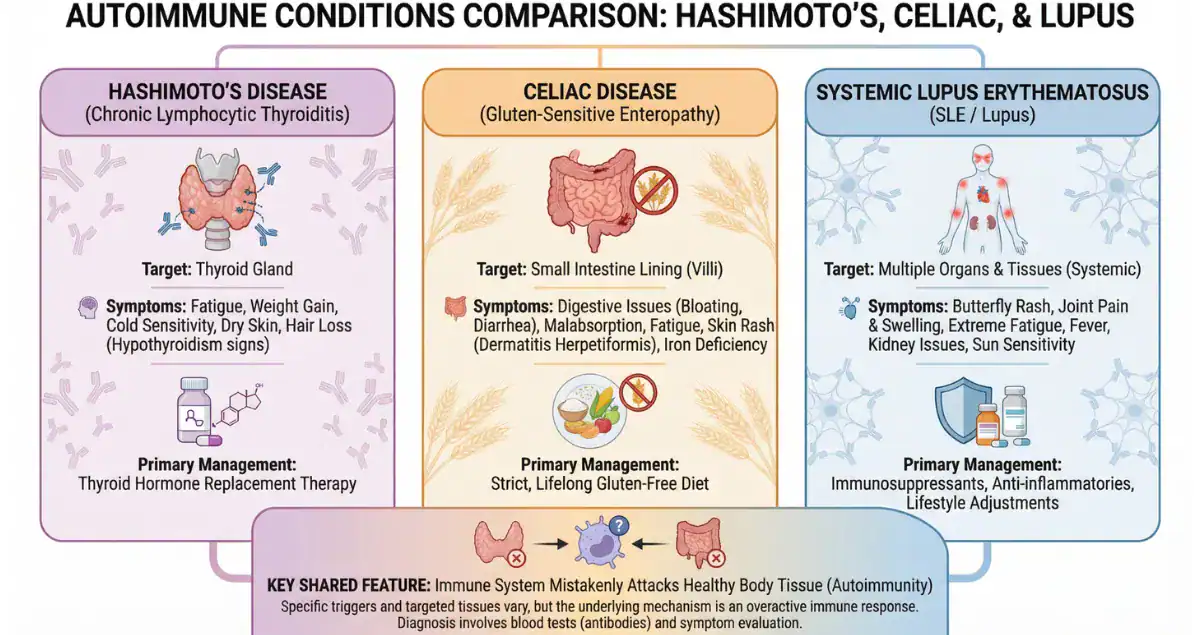
Autoimmune diseases occur when the immune system mistakenly targets the body’s own tissues, leading to chronic inflammation and organ damage. While these conditions are common, diagnosing them is often far from straightforward. Symptoms can overlap, laboratory findings may be nonspecific, and disease presentations can vary widely from patient to patient.
This is where pathology, and specifically biopsy, plays an essential role. A tissue sample examined under the microscope can reveal patterns of inflammation and injury that are not visible through blood tests or imaging alone. These histologic findings often provide the clarity needed to confirm a diagnosis, guide treatment, and assess disease severity.
Among the many autoimmune conditions, three stand out as some of the most commonly encountered in clinical practice: Hashimoto thyroiditis, celiac disease, and systemic lupus erythematosus. Each affects different organs, presents in unique ways, and relies on biopsy in distinct but important ways.
Hashimoto Thyroiditis: When the Immune System Targets the Thyroid
Hashimoto thyroiditis is one of the most common autoimmune diseases worldwide and a leading cause of hypothyroidism. It occurs when the immune system attacks the thyroid gland, gradually impairing its ability to produce hormones that regulate metabolism.
From a diagnostic standpoint, many cases are identified through blood tests showing elevated thyroid-stimulating hormone and the presence of anti-thyroid antibodies. However, biopsy becomes particularly important when imaging reveals thyroid nodules or when the clinical picture is unclear.
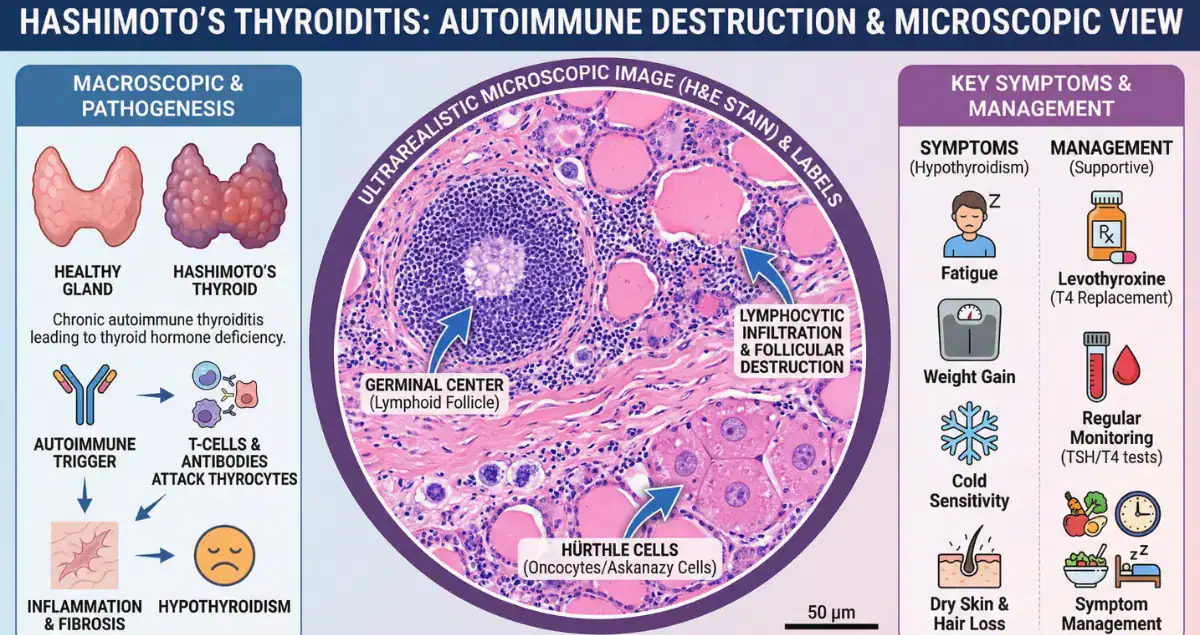
Histologically, Hashimoto thyroiditis is characterized by dense lymphocytic infiltration of the thyroid parenchyma. These lymphocytes often form germinal centers, and the normal thyroid follicles become disrupted and atrophic. Another hallmark feature is the presence of Hürthle cell change, where thyroid epithelial cells develop abundant granular cytoplasm.
A common concern is whether this condition increases the risk of cancer. While most cases are benign, there is a slightly increased risk of certain lymphomas of the thyroid. In such scenarios, biopsy is essential to distinguish between reactive lymphoid infiltration and malignant transformation.
For patients reviewing their pathology reports, the presence of lymphocytes in the thyroid can be confusing or alarming. Clear interpretation is key to understanding that, in most cases, this reflects a chronic autoimmune process rather than malignancy.
 Celiac Disease: Small Intestinal Damage Revealed by Biopsy
Celiac Disease: Small Intestinal Damage Revealed by Biopsy
Celiac disease is another highly prevalent autoimmune condition, triggered by an immune response to gluten in genetically susceptible individuals. It primarily affects the small intestine, leading to malabsorption and a wide range of gastrointestinal and systemic symptoms.
While blood tests for specific antibodies are often used as an initial screening tool, biopsy of the small intestine remains the gold standard for diagnosis in many cases. This is because serologic tests can sometimes be inconclusive or affected by dietary factors.
Under the microscope, the classic findings include villous atrophy, crypt hyperplasia, and increased intraepithelial lymphocytes. The normally tall, finger-like projections of the small intestine become blunted or flattened, reducing the surface area available for nutrient absorption.
Patients often ask whether a biopsy is always necessary for diagnosis. In some pediatric cases with strong clinical and serologic evidence, guidelines may allow for diagnosis without biopsy. However, in adults, histologic confirmation is typically recommended to ensure accuracy.
Biopsy also plays a role in monitoring disease progression or response to a gluten-free diet, particularly in patients with persistent symptoms. It helps distinguish between ongoing autoimmune activity and other potential causes of gastrointestinal distress.
Systemic Lupus Erythematosus: A Multisystem Disease with Variable Findings
Systemic lupus erythematosus is a complex autoimmune disease that can affect multiple organs, including the skin, kidneys, joints, and nervous system. Its presentation is highly variable, making diagnosis particularly challenging.
Unlike Hashimoto thyroiditis or celiac disease, lupus is not defined by a single organ or biopsy site. Instead, tissue sampling is often targeted to the organ most affected by the disease. Among these, kidney biopsy is one of the most critical.
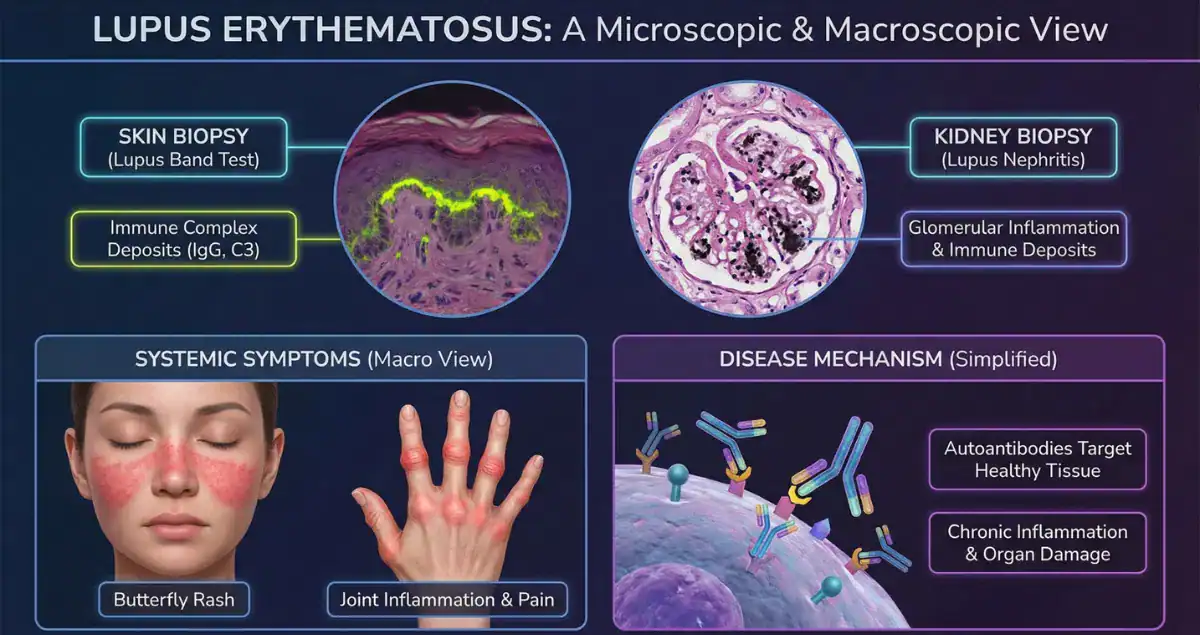
In lupus nephritis, biopsy provides essential information about the type and severity of kidney involvement. Histologic patterns are classified into different categories, each with specific treatment implications. Findings may include immune complex deposition, inflammation of the glomeruli, and varying degrees of scarring.
Skin biopsy is another useful tool in lupus, especially in cases with cutaneous manifestations. Histology often shows interface dermatitis, with lymphocytes targeting the dermoepidermal junction. Additional features such as basement membrane thickening and dermal mucin deposition can support the diagnosis.
A common question is whether lupus can be diagnosed without biopsy. In many cases, diagnosis is based on a combination of clinical features and laboratory findings. However, biopsy becomes essential when assessing organ involvement, particularly in the kidneys, where treatment decisions depend heavily on histologic classification.
 What Role Does Biopsy Really Play in Autoimmune Disease?
What Role Does Biopsy Really Play in Autoimmune Disease?
Biopsy is not always the first step in diagnosing autoimmune disease, but it is often the most definitive. It provides direct evidence of how the disease is affecting tissue at a microscopic level. This can confirm a suspected diagnosis, rule out other conditions, and provide prognostic information.
Patients frequently wonder whether biopsy results can change over time. The answer is yes. Autoimmune diseases can evolve, and repeat biopsies may be necessary in certain situations to reassess disease activity or response to treatment.
Another common concern is whether biopsy findings are always clear-cut. In reality, interpretation can be nuanced. Overlapping features, sampling limitations, and early disease can make diagnosis challenging. This is why expert pathology review is so important.
Why Expert Interpretation Matters More Than Ever
As autoimmune diseases become better understood, the role of pathology continues to expand. Histologic findings are increasingly integrated with clinical and laboratory data to create a more complete picture of disease.
However, pathology reports are often written in highly technical language that can be difficult to interpret. Terms like “lymphocytic infiltration,” “villous atrophy,” or “immune complex deposition” carry significant meaning but are not always self-explanatory.
This is where services like Honest Pathology can provide real value. By offering clear, detailed explanations of pathology findings, Honest Pathology helps patients and clinicians better understand what a biopsy result actually means. Rather than navigating complex terminology alone, individuals can gain insight that supports informed decision-making and more confident discussions with their healthcare providers.
Gaining Clarity and Confidence in Your Diagnosis
Autoimmune diseases can be overwhelming, especially when diagnosis involves multiple tests and unfamiliar terminology. Biopsy often serves as a turning point, providing concrete evidence that helps guide the next steps in care.
Understanding the role of biopsy in conditions like Hashimoto thyroiditis, celiac disease, and systemic lupus erythematosus can make the diagnostic process feel more manageable. It highlights how microscopic findings translate into real-world implications for treatment and prognosis.
For those seeking additional clarity, Honest Pathology offers a trusted resource to help interpret complex reports and bring meaning to the details. In a field where precision matters, having access to clear and reliable explanations can make all the difference in moving forward with confidence.