A lung cancer diagnosis often comes with unfamiliar and intimidating terminology. Among the most common and confusing distinctions patients encounter is whether their cancer is classified as adenocarcinoma or squamous cell carcinoma. While both are types of non–small cell lung cancer, they differ in how they develop, how they behave, and how they are treated. Understanding these differences can help patients make sense of their pathology report and better engage in conversations about care.
Why Lung Cancer Subtypes Matter
Lung cancer is not a single disease. It includes multiple subtypes that arise from different kinds of cells within the lung. Identifying the exact subtype is one of the pathologist’s most important tasks, because treatment decisions increasingly depend on these distinctions.
Adenocarcinoma and squamous cell carcinoma together account for the majority of non–small cell lung cancers. Although they may share symptoms and appear similar on imaging, they are biologically distinct diseases with different risk factors, molecular features, and therapeutic options.
What Is Lung Adenocarcinoma?
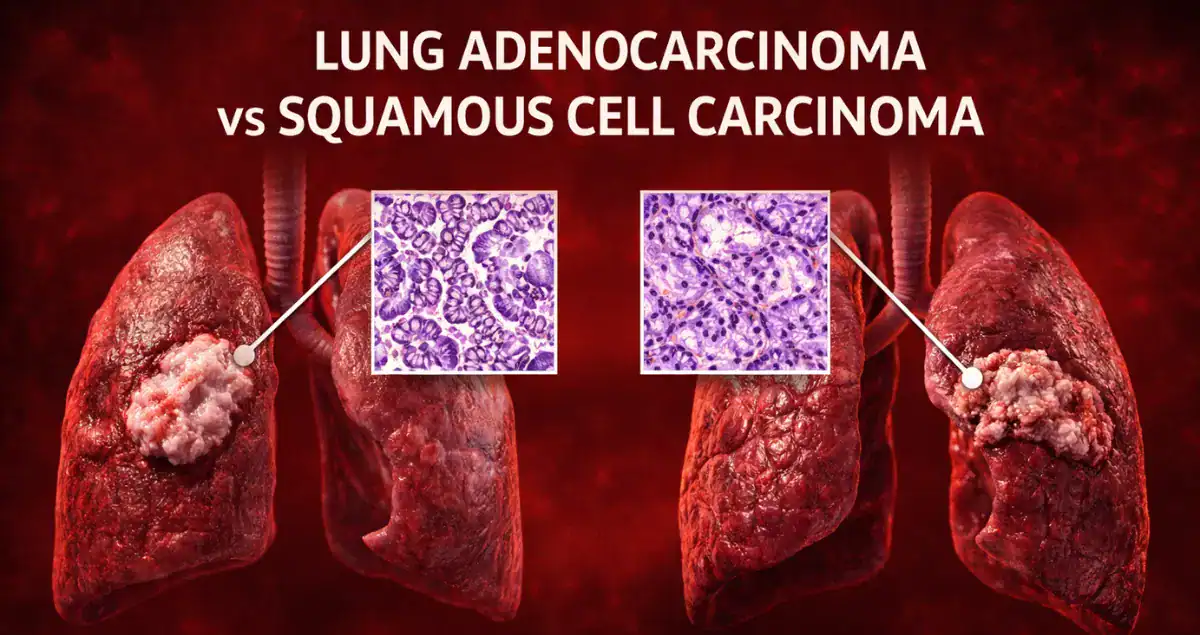
Adenocarcinoma of the lung develops from glandular cells that line the airways and produce mucus or other secretions. These tumors most commonly arise in the outer, or peripheral, regions of the lung rather than near the central airways.
Adenocarcinoma is the most common type of lung cancer overall and is particularly common in people who have never smoked or who smoked lightly in the past. It is also more frequently diagnosed in women compared to other lung cancer subtypes.
Under the microscope, adenocarcinomas show gland-like structures or cells that produce mucus. Pathologists may further classify adenocarcinoma into patterns such as lepidic, acinar, papillary, micropapillary, or solid, which can carry prognostic significance.
What Is Squamous Cell Carcinoma of the Lung?
Squamous cell carcinoma arises from squamous cells, which are flat cells that normally line the larger airways of the lung. These tumors are more often found in the central parts of the lung, near the bronchi.
Squamous cell carcinoma has a strong association with smoking and is more common in individuals with a significant smoking history. Historically, it was the most common type of lung cancer, though its relative frequency has declined as smoking patterns have changed.
Microscopically, squamous cell carcinomas show features such as keratin formation and intercellular bridges, which help pathologists distinguish them from other lung cancer types.
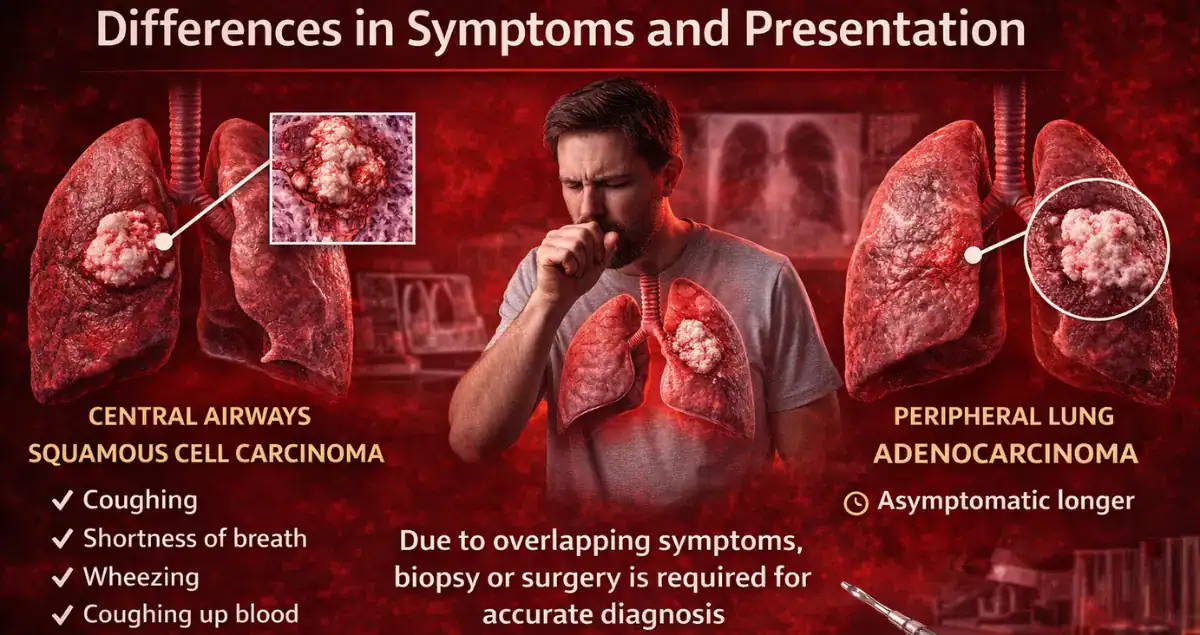
Because squamous cell carcinomas tend to arise in central airways, they may cause symptoms earlier, such as coughing, wheezing, shortness of breath, or coughing up blood. Adenocarcinomas, which often grow in the peripheral lung, may remain asymptomatic longer and are sometimes discovered incidentally on imaging.
Despite these tendencies, symptoms can overlap significantly, and imaging alone is not sufficient to reliably distinguish between these subtypes. Tissue diagnosis through biopsy or surgery is required.
Molecular Differences and Targeted Therapy
One of the most important differences between adenocarcinoma and squamous cell carcinoma lies at the molecular level. Lung adenocarcinomas are much more likely to harbor genetic alterations that can be targeted with specific therapies. These may include mutations in genes such as EGFR, ALK, ROS1, BRAF, KRAS, and others.
Because of this, molecular testing is routinely recommended for adenocarcinoma and for many non–small cell lung cancers with adenocarcinoma features. Identifying these mutations can open the door to targeted treatments that may be more effective and better tolerated than traditional chemotherapy.
Squamous cell carcinomas, in contrast, are less likely to have these targetable mutations. While molecular testing may still be performed in certain cases, especially in patients with limited smoking history, treatment options for squamous cell carcinoma more often rely on chemotherapy, radiation, and immunotherapy.
Differences in Treatment Approaches
Treatment decisions for lung cancer depend on many factors, including stage, overall health, and patient preferences. However, histologic subtype plays a key role.
Adenocarcinoma patients are more likely to receive targeted therapies if a relevant mutation is identified. These therapies can significantly alter prognosis and quality of life. Squamous cell carcinoma patients may have fewer targeted options but can respond well to immunotherapy, sometimes in combination with chemotherapy.
Certain drugs are avoided in squamous cell carcinoma because of higher risks of complications, underscoring why accurate classification is critical.
Prognostic Considerations
Prognosis varies widely within both adenocarcinoma and squamous cell carcinoma, depending on stage at diagnosis and response to treatment. In general, adenocarcinoma has a broader range of outcomes because of its molecular diversity and the availability of targeted therapies.
Squamous cell carcinoma may present earlier due to symptoms but can also be more locally aggressive. These generalizations do not predict individual outcomes, which is why personalized evaluation is essential.
The Role of Pathology in Making the Distinction
Distinguishing adenocarcinoma from squamous cell carcinoma is a central task for the pathologist. In small biopsies, the distinction can be challenging, especially when tumors are poorly differentiated. In these cases, immunohistochemistry is often used to confirm the subtype by highlighting proteins characteristic of glandular or squamous differentiation.
Accurate classification ensures that patients receive appropriate molecular testing and avoids treatments that may be ineffective or harmful for a particular subtype.
Why Diagnostic Accuracy Is So Important
Misclassification between adenocarcinoma and squamous cell carcinoma can have real consequences. It may lead to missed opportunities for targeted therapy, inappropriate testing, or suboptimal treatment choices. Because of this, expert pathology review can be particularly valuable in lung cancer, especially when the diagnosis is made on a small biopsy or when treatment decisions are complex.
Empowerment Through Understanding
Learning the difference between adenocarcinoma and squamous cell carcinoma can help patients better understand their diagnosis and the rationale behind recommended treatments. While the terminology can feel overwhelming at first, clarity about cancer subtype often brings a greater sense of control and confidence during decision-making.
For patients seeking deeper understanding or confirmation of their lung cancer diagnosis, Honest Pathology offers independent expert pathology review and clear, patient-focused explanations. Their goal is to help patients fully understand what their pathology report means so they can move forward with informed and confident choices about their care.